Cigna and The Hospital of Central Connecticut say they could sever ties next month if they can’t reach a new contract agreement–the latest in a string of public contract disputes between hospitals and insurers.
Each dispute has its own dynamics, but experts say the spate of contentious contract negotiations reflects the uncertainties hospitals and insurers face from health reform and the down economy.
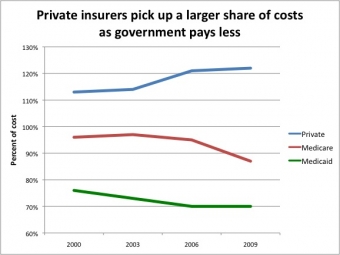
It’s also a symptom of the increased pressure on private insurance to cover the costs that government health care programs like Medicare and Medicaid do not. For every dollar of cost they incurred in 2009, Connecticut hospitals were paid 87 cents by Medicare and 70 cents by Medicaid–and $1.22 by private insurance, according to the state Office of Health Care Access.
The so-called cost shift from government payers to the private sector is not a new phenomenon. But the model has been facing increased pressures, leading some to question whether it can be sustained.
In Connecticut, Medicaid enrollment has boomed since the recession began in March 2008; enrollment in the HUSKY health plan, which covers mostly low-income children and their parents, rose more than 21 percent to nearly 406,000 people this month, and other Medicaid programs have also enrolled more people. Medicare rolls are poised to rise as baby boomers begin turning 65, leaving hospitals with even more patients whose care is delivered at a loss.
The employers who pay for the private insurance that helps cover government shortfalls, meanwhile, are increasingly struggling to afford coverage, putting more pressure on insurers to keep rates down. And health reform is expected to add more than 100,000 people to Connecticut’s Medicaid program.
“We are looking at what the implications of that are and how that’s going to take a situation which was very difficult to manage in the past and essentially make it one which is unbearable,” said Stephen A. Frayne, senior vice president for health policy at the Connecticut Hospital Association. “Particularly when it’s linked to a state budget which has fairly significant problems.”
Coverage and Cost Shift
The majority of Connecticut residents are still covered by private health insurance, although census estimates indicate that the proportion of the insured with private coverage dropped between 2008 to 2009, from 78.4 percent to 76.2 percent.
But hospitals see patients with Medicare and Medicaid more often. In 2009, people covered by public programs accounted for more than half of patient encounters at hospitals, according to the Office of Health Care Access.
Health reform could add 114,000 or more people to the state’s Medicaid program by 2019. Because the newly covered will largely be people who would otherwise be uninsured, some hospital officials expect it will lead to a drop in their costs for uncompensated care, although Frayne said hospitals will still have trouble keeping up with the cost of caring for the newly covered.
In addition, some of the people receiving coverage in 2014 could require extensive medical care to address health problems that might not have gotten adequate medical attention while they were uninsured.
Frayne said he and others are looking at ways for the state to access federal money to help subsidize the cost of government coverage, which could allow the state to raise the rates paid to health care providers. One example he cited is a plan in the SustiNet proposal, which would create a state-run insurance program, to use federal funds to create a “basic health plan” for people whose incomes fall just above Medicaid eligibility, and use some of the money to increase provider rates.
Not everyone agrees that the higher costs commercial insurers pay to hospitals can be blamed on government underpayment. The Medicare Payment Advisory Commission, or MedPAC, which advises Congress on Medicare issues, has argued that Medicare payments are adequate for relatively efficient hospitals, and that raising Medicare rates would not necessarily lead to lower commercial charges. Hospitals that make high margins from commercial payers have less pressure to rein in costs, the group has argued, leading to expenses beyond what Medicare pays.
The actuarial firm Milliman concluded that a cost shift did exist in a 2008 analysis prepared for insurers and hospitals. The firm estimated the cost shift nationwide at $88.8 billion per year, or about 15 percent of what commercial insurers spend on hospital and physician services. The report defined cost shift as the difference between actual payments and payment amounts that would produce equal margins for each payer.
But more recent Milliman research has suggested that cost shifting is not the only option for hospitals, and that they might have little choice in the future but to become more efficient. The firm identified cities that have “high-value” hospital care, with low per capita inpatient costs for both Medicare and commercial insurance, and positive hospital margins.
“Considering cost shifting to be inevitable ignores both the potential for cost management within hospitals and hospitals’ flexibility to set commercial prices,” one report said. “The data demonstrates that hospitals can prosper in some low-Medicare cost regions without cost shifting to commercial payers for their inpatient services.”
Fundamental Change
With employers struggling to pay higher insurance rates and hospitals treating more people with government-sponsored or no insurance, some hospital and insurance industry officials are looking to other models.
“We feel that there needs to be some sort of fundamental change in how things are paid for,” said Martha Temple, President of the New England Market for Aetna.
“There’s just no more ability to sustain that model,” said Bristol Hospital President and CEO Kurt Barwis. Bristol Hospital stopped accepting United Healthcare briefly during a 2009 contract dispute, and went through more of a year of negotiations and clashes with Anthem Blue Cross and Blue Shield before finalizing contracts last year.
Bristol Hospital, like many of its counterparts, has been working to become more efficient, looking to strategies that have worked in other industries, like supply chain management.
Hospitals are also devoting increased attention to measuring and reporting patient outcomes, and are working to make improvements such as reducing the number of patients who are readmitted soon after being discharged. Beginning next year, the federal government will reduce payments to hospitals for preventable hospital readmissions.
Such changes can ultimately save money and improve care, but getting there can take time and money, putting even more pressure on hospitals already facing tight margins.
“It’s a very dynamic time, and I don’t know of any CEO that’s not working at the quality-cost focus, how can we deliver better outcomes, better quality at a lower cost,” Barwis said.
At Hartford Hospital, officials are focusing on changes such as reducing readmissions and bloodstream infections, which drive up costs. The efforts are aimed at improving the quality of care and its cost, regardless of what the future payment structure looks like, Executive Vice President and Chief Operating Officer Jeffrey Flaks said.
Hartford Hospital and its affiliates have been through contentious contract negotiations with Anthem and Aetna over the past two years. Flaks said the nature of negotiations remains similar to previous talks, but with a somewhat different focus.
“I do think there is a greater focus around value,” Flaks said.
Aetna is using pay-for-performance agreements with hospitals and large physician groups, with targets such as reduced hospital readmissions or making sure patients get appropriate screenings. Temple said providers appear eager to discuss delivery system changes.
Performance incentives can help in contract negotiations, Temple said, but cost shifting will always be an issue.
Hospitals delivering better outcomes more cost-effectively will be good for everyone, Barwis said. But the economic gains from it could be offset by continued cost shifting from expanded government programs. And it’s not clear what it could mean for future commercial insurance contracts.
“I don’t think anyone has a crystal ball that predicts whether it’s enough to improve or end what appears to be a much more contentious payer, provider negotiation environment,” he said.



