NEWINGTON–Gina Corraccio set up her laptop on Frank Silva’s kitchen table and began quizzing her patient. What had he cooked in the past week? Was he having trouble with routine activities, like making the bed? And why had he been gaining weight?
Ever since Silva got out of the hospital in January, part of Corraccio’s job as a visiting nurse has been to stay on top of his health. Silva, 87, has diabetes and unstable angina, and in the past year, had been something of a regular hospital patient, getting admitted for inpatient care every couple months.
This visit marked something of a milestone: more than 60 days since Silva had come home from the hospital, with no inpatient stays since.

Nurse Gina Corraccio checks in on Frank Silva at his Newington home
But the weight gain, an indicator of problems in heart failure patients, could threaten that streak. Silva suspected it was from being taken off one of his water pills. Corraccio examined his blood work and made a note to check with the doctor who made the change.
“I’ll follow up,” she said.
The effort to keep Frank Silva out of the hospital is part of a large-scale move to change the way patients are cared for after discharge. How well it works will have implications for far more than Silva and patients like him.
Nationally, more than one in four Medicare patients hospitalized for heart failure were back in the hospital within 30 days of being discharged, according to a study of 2003 and 2004 data published in the New England Journal of Medicine in 2009. More recent data for patients at Connecticut hospitals show similar rates.
That comes at a cost. Unplanned rehospitalizations accounted for $17.4 billion in Medicare spending, or nearly 17 percent of Medicare payments to hospitals, in 2004, the authors of the New England Journal article found. Potentially preventable readmissions account for about $12 billion in annual Medicare spending, according to the Medicare Payment Advisory Commission, which advises Congress on Medicare policy.
Part of the problem is the complexity of conditions like congestive heart failure. But much of it also stems from the lack of coordination in the health care system, and a payment structure that does little to encourage anyone to fill the gaps.
Until recently, hospitals had little financial incentive to worry about what happened to patients once they left the building. Hospitals get paid when patients come in, whether it’s the result of a new problem or a return visit.
But the focus is starting to change. Under the federal health reform law, hospitals will receive reduced Medicare payments if they are deemed to have too many preventable readmissions for patients with heart failure, heart attacks and pneumonia. Hospitals are also anticipating a move toward bundled payments, which would pay them a certain amount for an “episode of care”–a period lasting from just before admission to 30 days after discharge, for example–rather than a separate fee each time the patient visits or gets admitted.
That’s led hospitals to focus on reducing readmissions, an effort that requires coordinating with other providers who care for patients after discharge, including private physicians, nursing homes and home health agencies.
“It’s not an incentive to put the patient in the hospital,” said Dr. Richard J. Soucier, medical director of the congestive heart failure service at St. Francis Hospital and Medical Center, and Silva’s cardiologist. “It’s going to be an incentive to keep them out.”
Reducing readmissions also means tackling the reasons why patients don’t always do what doctors tell them.
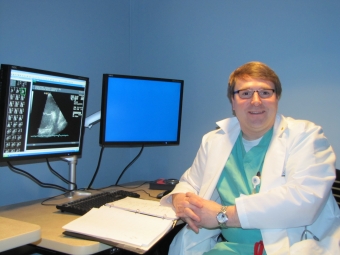
Dr. Richard Soucier was surprised to learn what patients don’t tell him
In Silva’s program, a partnership between St. Francis and Masonicare Partners Home Health & Hospice, visiting nurses like Corraccio help translate doctors’ instructions to patients’ lives. Sometimes that means taking a patient grocery shopping to demonstrate how to build a low-sodium diet, which is critical for heart failure patients.
Soucier has been struck by how much more willing patients can be to discuss life stresses that can affect their health with people who aren’t doctors.
“I’m surprised at how intimidating I am,” he said. “I’m surprised at how difficult it is for people to broach certain subjects with me versus with the people who I have on my staff.”
He’s also learned not to take certain things for granted, like the idea that patients understand what salt is or comprehend his instructions.
“I had a guy, I wrote a prescription out for meds and I explained to him how I wanted him to take them and wrote it down,” Soucier said. “And he couldn’t read. But he didn’t tell me that.”
Micromanaging
Silva went to St. Francis last fall after having a heart attack. He was discharged to a nursing home to recover, but he quickly began gaining weight, which can indicate that the body is retaining extra fluid and the heart failure is worsening. The doctors at the nursing home didn’t communicate with his regular doctors, Silva said. Soon after, he was back in the hospital.
He got out again in January, and insisted on going home to the house he had built for his family in 1977.
Among the things that can land a heart failure patient back in the hospital are not keeping up with an extremely low-sodium diet and not taking medications as prescribed. Neither is easy. Silva takes 13 or 14 medications, and that puts him on the low end. The average heart failure patient takes 18 prescription drugs, Soucier said. The regimen can get more confusing after a hospitalization because patients are often given different medications in the hospital and don’t know which ones to take when they get out.
Patients tend to get some education on how to take their medications and eat right while they’re in the hospital. But people don’t always retain much of the information they get in an environment that’s far removed from home and often filled with distractions like beeping monitors.
“So they go home and have no idea what the heck it is that you told them to do with sodium and how to exercise and any of that,” Soucier said.
A patient having a problem might make an appointment to see the doctor. But by the time it comes, two or three weeks later, the patient could be just as sick as he was in the hospital.
“So what we’ve tried to do is intercede up front,” Soucier said.
In the program, a Masonicare nurse begins working with patients when they’re still in the hospital. Once they leave, a nurse visits the patients at home within 24 hours. Each patient will get two more visits that week, and have an appointment at Soucier’s clinic within three days, where a disease management nurse will reconcile the patient’s medications.
Patients are also monitored daily through a telemonitoring device. It has a scale, blood pressure cuff and an oxygen sensor and is hooked up to a landline telephone. Silva uses it every morning to take his vitals, which get transmitted to nurses who can relay any problem to his medical team. That’s how Corraccio knew about the weight gain.
“Anytime something’s wrong, I get a call on the phone,” Silva said. “They get right back on my case.”
Katie Leahy, Masonicare’s cardiac transition coordinator, likes to use the term “micromanage” to describe what the program does for patients.
“We stay on top of them and really try to micromanage them,” she said. “I always say that word, but that’s really what needs to happen.”
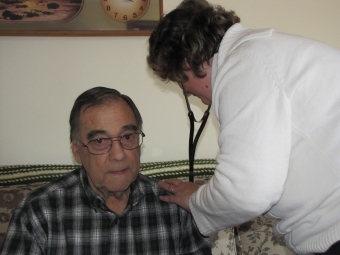
Heart Failure Nurse Holly Wills listens to Frank Silva breathe during a visit earlier this month
The Masonicare program has been small, with 111 patients between April 2009 and April 2010. But the results are promising, with 12 percent of the patients readmitted within 30 days, just under half the national average.
Some patients find the home visits too invasive. Some prefer fewer visits or to skip the telemonitoring, which Leahy said they will accommodate. If a patient in the program is readmitted to the hospital, the nurses often have insights into why.
Reading Labels
Corraccio says education is key–making sure patients understand how their eating habits affect their conditions, how heart failure works and what the signs of problems are.
One of the first things she likes to ask new patients to do is to get a can from the pantry and read the nutrition label. Often, they can’t, or they don’t read it correctly.
Silva acknowledges he was one. He could read the labels, but didn’t recognize that the information applied to one serving, not the entire container.
Limiting salt intake is usually a challenge, especially for those who live alone, like Silva, whose wife of 59 years died. Silva’s children visit and have him over for meals, but Corraccio said patients’ family members generally aren’t able to make low-sodium meals, and microwavable or canned foods tend to be high in sodium.
Silva has it doubly hard; his diabetes requires him to avoid sugar too. But he’s getting more adept at managing his diet and reading up on his options. When Corraccio arrived for her recent visit, Silva showed her a hardcover he got called “The Salt Solution.” “That’s my salt-free book,” he said.
“If you stay away from salt, I’m fine,” he said. “That’s what it’s telling me.”
Corraccio’s visit to Silva was one of the last covered by Medicare. He will continue to receive nursing visits through a state program and will maintain the telemonitoring.
“She’s given me all kinds of information,” he said as Corraccio wrapped up her visit. “She’s helped me tremendously.”


