Several key provisions of the federal health reform law known commonly as Obamacare are taking effect Jan. 1.
For some people, like the uninsured, that will bring major changes. For many others, like those who get their insurance through their jobs, not much will change.
Here’s a look at how various groups of people will be affected, what their insurance options are now and what choices they’ll have beginning in 2014.
The Young Invincible: Different choices and a potential penalty
Example: 28-year-old, no kids, two part-time jobs, no health benefits
Annual income: $40,000
Current options: He can buy coverage through the state’s individual insurance market. Or, like many people his age, he might choose to go without insurance.
As of Jan. 1: He’ll be required to have health insurance, or face a penalty (about $300 next year; the fine is $95 or 1 percent of income, whichever is higher. It will go up in 2015).
- He’ll still be able to buy coverage through the state’s individual market. But some plans he might currently consider, like very inexpensive plans with very high deductibles or limited coverage, will no longer be available because the health law requires that plans sold directly to individuals cover a set of essential health benefits and limit out-of-pocket costs to $6,350 for an individual.
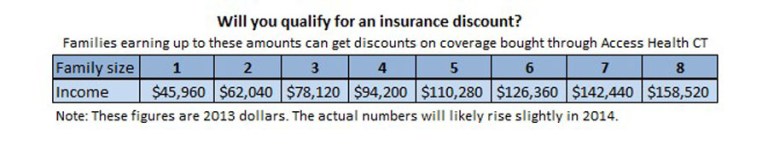
- A new option: He could buy insurance through Access Health CT, the state’s health insurance exchange, a marketplace created by the health reform law. Because his income is less than 400 percent of the poverty level, he’ll qualify for a discount on his monthly premiums if he buys coverage through Access Health.
- Because he’s under 30, he’s eligible to buy a catastrophic plan through Access Health that provides very limited coverage and has a high deductible, but lower premiums than more comprehensive coverage. Unlike many catastrophic plans sold now, it will be required to cover the same essential health benefits that other plans do once he hits the deductible. It must also cover at least three primary care visits a year, even if he hasn’t reached the deductible, and certain preventive services with no charge.
If…he were under 26, he’d also be eligible for coverage through his parents’ insurance.
The Low-Income Couple: Newly Medicaid eligible
Example: Husband and wife, both 32, no minor children, part-time jobs, no insurance
Annual income: $20,000
Current options: This couple is above the current threshold for Medicaid. They can buy insurance through the state’s individual market or the state’s Charter Oak Health Plan.
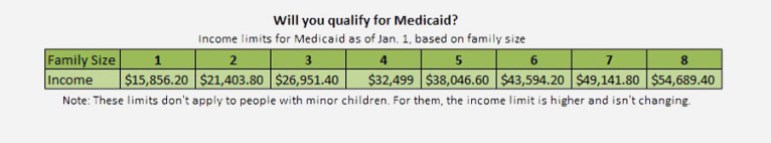
As of Jan. 1: They’ll be eligible for Medicaid. As part of the health reform law, Connecticut is expanding Medicaid to adults earning up to 138 percent of the poverty level. Between 55,000 and 60,000 adults are expected to become eligible.
If…this couple had minor children, they’d already be Medicaid eligible. Connecticut’s Medicaid program covers adults with minor children earning up to 185 percent of the poverty level. That won’t change.
A Pre-Existing Condition: New Options
Example: Woman, 45, with multiple sclerosis and no employer-sponsored insurance
Annual income: $50,000
Current options: People with pre-existing conditions have a hard time buying coverage through the state’s individual insurance market because insurers can deny coverage or charge higher rates based on their medical histories.
- The state operates a high-risk pool for people with pre-existing conditions. It’s run by the nonprofit Health Reinsurance Association and covers about 1,200 people. For this woman, the premium is about $1,189 per month.
- A temporary high-risk pool, the Connecticut Pre-Existing Condition Insurance Plan, costs $381 per month but is only available to people who’ve been without insurance for at least six months. (Enrollment in the program is closed, so it’s only an option for people who’ve already signed up.)
- The state’s Charter Oak Health Plan is accepting people with pre-existing conditions through December. Premiums are $589 per month.
As of Jan. 1
- She’ll be able to choose a plan sold on the individual market or through Access Health, the state’s health insurance exchange, because Obamacare will prohibit insurers from denying coverage or charging more based on a person’s medical history. (The extent to which this raises the cost of insurance for the overall population remains to be seen.)
- The Health Reinsurance Association high-risk pool will continue to offer coverage as it does now.
- The Connecticut Pre-Existing Condition Insurance Plan will no longer be available.
- Charter Oak won’t be available anymore either.
Higher Income, Uninsured: No Help Buying Coverage
Example: Husband, 50, wife 45, both self-employed; two teenage kids
Annual income: $98,000
Current options
- They could buy insurance through the state’s individual insurance market.
- They could also get their kids covered by the state’s HUSKY B program, which would cost them $314 per month per child (it’s subsidized for people with lower incomes).
- They could go without insurance.
As of Jan. 1
- They’ll still be eligible to buy coverage through the individual market and, for their kids, get HUSKY B.
- They could also buy coverage through Access Health CT, the state’s health insurance exchange. Because their income is over 400 percent of the poverty level, they won’t qualify for any subsidies to help pay for their coverage. Depending on where they live, the monthly premiums for the least expensive plans on the exchange could cost between $888.29 (Hartford County) and $1,290.88 (Fairfield County).
- If they go without insurance, they’d have to pay a $780 penalty.
49,000 of the uninsured people in Connecticut are expected to be ineligible for discounts on insurance because their income is too high.
The College Student: Not much changing
20-year-old in college
Current options: Students can buy coverage through their colleges or universities, get covered through their parents’ plans (up to age 26), or buy their own coverage through the state’s individual market. If their incomes are low enough, they could qualify for Medicaid. Or they can go without insurance.
As of Jan. 1: All of the previous avenues for getting coverage are still available, although some very low-cost, low-benefit health plans won’t be allowed to be sold anymore.
- College insurance plans satisfy the individual coverage mandate that takes effect Jan. 1.
- One change: If students go without insurance, they’ll face a financial penalty — but only if they earn enough money to pay income taxes (around $10,000). If not, they’re exempt from the mandate.
- Students can also buy insurance through Access Health CT, the state’s new insurance marketplace, or potentially qualify for Medicaid, if their income is low enough.
Employer-Sponsored Coverage: Not much changing
Example: Husband, 50, wife, 48, both covered through their employers
Current options: Like the majority of Connecticut residents with health insurance, they get their coverage through their employers.
As of Jan. 1: Employer-sponsored coverage fulfills the individual mandate, so they won’t face a penalty.
- Some aspects of their insurance coverage could change, depending on the size of the company and the way the employer handles its health plan. The changes include the types of benefits covered (plans sold to small businesses must cover a set of “essential health benefits”) and out-of-pocket limits (individuals’ costs for deductibles, copays and coinsurance will be capped at $6,350, and families’ costs will max out at $12,700; premiums don’t count toward those totals). In general, people who get their coverage through large employers will probably see the least amount of change because the types of plans common among big companies are exempt from some provisions of the health law and are likely to already meet other requirements.
One on Medicare, one without coverage
Example: Husband, 67, has Medicare. Wife, age 62, doesn’t get insurance through her job
Annual income: $60,000
Current options
- The man gets Medicare.
- The woman, who must buy her own health insurance, can buy it through the state’s existing individual market. She could also buy coverage through the state’s Charter Oak Health Plan.
As of Jan. 1:
- Nothing will change for the husband, who will still receive Medicare coverage.
- The wife can continue to buy insurance through the state’s individual market. Like other people who buy coverage on their own, she’ll also have a new option: buying coverage through Access Health CT, the health insurance exchange. Because their income is below 400 percent of the poverty level, she’ll qualify for a discounted rate if she buys coverage through Access Health.
- Charter Oak is being eliminated, so that option is off the table.
If…they earned more than 400 percent of the poverty level ($62,040 for a couple), she could still buy insurance on or off the exchange, but wouldn’t get any help paying the premiums on exchange plans.