Medicaid, the health care program for people who are poor or have disabilities, plays a key role in expanding coverage as part of the federal health reform law.
The scope of the changes to Connecticut’s Medicaid program is likely to be smaller than in many other states, because this state got a head start, expanding Medicaid shortly after the health law passed in 2010. Still, Connecticut’s Medicaid program, known as HUSKY, will expand further as of Jan. 1, and existing members will see some changes.
And even people who are seeking private coverage through Access Health CT, the state’s health insurance exchange, might find that their children could end up in HUSKY.
Here are some key things to know about how the law commonly known as Obamacare affects Medicaid in Connecticut.
1. The four HUSKYs
First, some basics: Connecticut’s HUSKY program has four parts that together provide health care coverage to more than 634,000 state residents. This fiscal year, it’s projected to cost $5.1 billion.
HUSKY A is a Medicaid program that covers children, their parents and pregnant women. It’s the biggest part of the program, with more than two-thirds of the total HUSKY membership.
 HUSKY B covers kids whose parents earn too much money to qualify for Medicaid. It’s open to Connecticut children regardless of family income, but only those below certain income levels can receive free or subsidized coverage. It’s part of the federal Children’s Health Insurance Program, known as CHIP.
HUSKY B covers kids whose parents earn too much money to qualify for Medicaid. It’s open to Connecticut children regardless of family income, but only those below certain income levels can receive free or subsidized coverage. It’s part of the federal Children’s Health Insurance Program, known as CHIP.
HUSKY C provides Medicaid coverage for people with disabilities, low-income seniors who also have Medicare, and people receiving long-term care. The bulk of the state’s Medicaid spending funds nursing home and home care for people in this program.
HUSKY D is the state’s newest Medicaid program and covers adults who don’t have minor children. It began in 2010 when Connecticut became the first state in the country to expand Medicaid under Obamacare. It’s expanding as of Jan. 1 to cover people at higher income levels.
Most of the Medicaid changes related to Obamacare involve HUSKY D — that is, adults who don’t have minor children.
2. More people will be eligible for Medicaid starting in January.
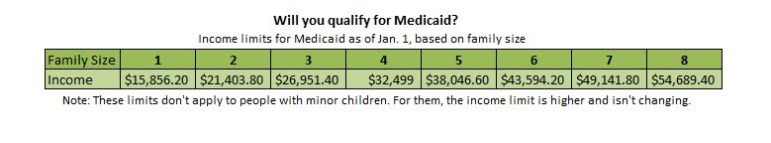
The income limit for Medicaid coverage for adults who don’t have minor children will increase Jan. 1 from 56 percent of the poverty level to 138 percent. That’s expected to add 55,000 to 60,000 people to the program.
People can enroll in the expanded Medicaid program through Access Health CT, the state’s health insurance exchange. Since the exchange opened last week, nearly half the people who have signed up for coverage will be Medicaid clients starting in January.
The income limit for HUSKY D will still be lower than the limit for children, parents and pregnant women to receive public coverage.
3. The application for families in HUSKY will get more complicated.
Right now, most people applying for HUSKY coverage can do so on a 4-page application. The relatively short form was the result of efforts in the 1990s to keep the process of seeking coverage as simple as possible.
But that form is being replaced because, as of Jan. 1, it won’t be considered enough to determine eligibility under new federal rules.
Instead, people using a paper application to apply for Medicaid coverage after Jan. 1 will need to use a longer form used to determine eligibility for both HUSKY and private coverage through the exchange. There are separate applications for individuals and families.
The impending change has frustrated advocates who have long tried to make applying for and renewing HUSKY coverage as straightforward as possible.
“In a state like Connecticut that’s made a lot of progressive changes in the Medicaid application procedure, some of the changes associated with the Affordable Care Act are a step backward,” said Mary Alice Lee, a senior policy fellow at Connecticut Voices for Children.
State officials say they have little choice in the matter and are basing the new application on a federal template.
People seeking Medicaid coverage for Jan. 1 — but who don’t want or don’t qualify for coverage sooner — can apply online now through Access Health’s website.
The state Department of Social Services is also developing an online application that people will be able to use to apply for Medicaid.
If people submit the 4-page application after Jan. 1, it will be accepted but considered incomplete, and applications will have to provide additional information.
4. Many families buying coverage through Access Health CT will end up with discounted private insurance for the parents and HUSKY for the kids.
The health reform law provides federal tax credits to discount the price of insurance for many people who buy coverage through the exchanges. But people who qualify for Medicaid aren’t eligible to receive those subsidies.
Connecticut’s income limit for HUSKY is higher for kids than for adults. So in some families, parents will qualify for subsidized private coverage while their children, who qualify for HUSKY B, won’t.
For those families, Access Health’s calculator will suggest the parents enroll in subsidized private coverage while the children sign up for HUSKY B.
People in that situation can choose to enroll their children in private coverage instead, but would have to pay the full price, which ranges from $125 to $293 per month depending on the county and coverage level.
This applies to families whose children qualify for subsidized HUSKY B premiums. The income limits for that coverage are:
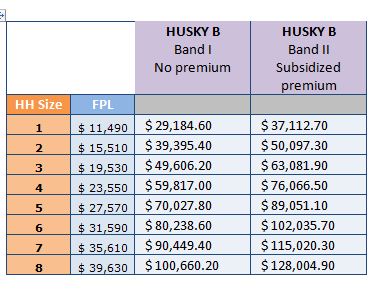
Experts say it’s not unusual for families to split coverage now, with adults covered by private plans and children in HUSKY B.
5. The HUSKY income calculations for children and families are changing.
Eligibility for families in HUSKY isn’t expanding like it is for adults who don’t have kids. But the way the program counts income is changing.
The vast majority of people currently in the program are expected to remain eligible, according to DSS. It’s not clear whether additional people will become eligible, although DSS said the federal government considers the change cost-neutral, indicating that a significant bump in enrollment is not anticipated.
Still, the new method for counting income could result in changes in eligibility for some families close to the limit.
Right now, families are eligible for HUSKY A if they earn up to 185 percent of the poverty level, and pregnant women are eligible at up to 250 percent of the poverty level. Other factors are taken into account, including child care costs and some child support payments, which reduce the amount of income counted in the eligibility calculation.
As of Jan. 1, the way income is counted will change as part of the federal health law. As a result, the HUSKY A and B income limits are rising.
Here are the old and new income limits:
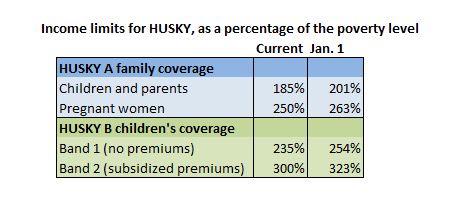
And here’s how the new limits translate in dollars:

6. The Medicaid program for people with disabilities and low-income seniors — HUSKY C — isn’t changing the way the other parts of HUSKY are.
Unlike the other HUSKY programs, the way income is calculated for HUSKY C isn’t changing. That means that people seeking HUSKY C coverage should apply through the state Department of Social Services, rather than through Access Health CT, the state’s health insurance exchange, according to DSS.
In some cases, people who are above the income limit for HUSKY C could qualify if their medical expenses exceed the amount by which they’re above the program’s income limit. They could be eligible for a “spend-down,” meaning that once they spend their additional income on medical costs during one six-month period, they can qualify for Medicaid for the remainder of the period.
People in those circumstances could also qualify to buy private insurance through Access Health at a discounted rate. Whether that ends up costing more or less than the Medicaid spend-down option depends on the person’s individual circumstances. Sheldon Toubman, an attorney with the New Haven Legal Assistance Association, advised people who might qualify for a Medicaid spend-down to apply both to DSS and Access Health to compare their options.
7. If you qualify for Medicaid now and want coverage before Jan. 1, you should apply through DSS, not the exchange.
Access Health determines eligibility for Medicaid using the rules that will take effect Jan. 1, not the method currently in use. So anyone who qualifies for Medicaid now and wants coverage immediately should apply through DSS to have his or her eligibility determined using the current rules, according to the department.