In its first 15 days of operations, Connecticut’s new insurance marketplace signed 3,847 people up for health care coverage as part of the law commonly known as Obamacare.
Most of the early customers were ages 55 to 64, and, among enrollees under 35, the majority will get Medicaid coverage. Two-thirds of those signing up for private insurance chose plans offered by the state’s largest insurer, Anthem Blue Cross and Blue Shield, and small businesses have lagged behind individuals in signing up, with only 11 submitting applications so far, according to data presented to the marketplace’s board Thursday.
The data was the most comprehensive presented so far, and according to CEO Kevin Counihan, is more than federal officials wanted states to release.
Unlike Connecticut, which chose to develop and run its own marketplace known as a health insurance exchange, 34 states have exchanges that are run fully or in part by the federal government. The federal government has faced criticism for its handling of those exchanges, including not reporting how many people have enrolled so far.
“Technically speaking, we’re releasing more information to the board today than CMS would typically want us to do,” Counihan said, referring to the federal Centers for Medicare and Medicaid Services.
According to the data from Connecticut’s exchange, known as Access Health CT, 10,768 applications were started between Oct. 1 and Oct. 15, and just over one in five — 2,372 — were completed. Because some applications cover families, the number of total people signed up is larger than the number of applications.
Enrollment for coverage through Access Health opened Oct. 1. People have until March 31 to sign up for insurance coverage in 2014, but those who want the coverage to start Jan. 1 — the first day it will be available — must apply by Dec. 15. In addition, to avoid facing a penalty for being uninsured for more than 90 days, people must apply by Feb. 15, since coverage takes effect on the first day of the following month.
Exchange officials hope to sign up 100,000 people in the first year of operation.
Access Health offers insurance plans sold by private insurers. Many customers are expected to qualify for federal tax credits to discount their premiums. People can also use Access Health to apply for coverage through the state’s Medicaid program, which is expanding Jan. 1 to cover more adults who don’t have minor children.
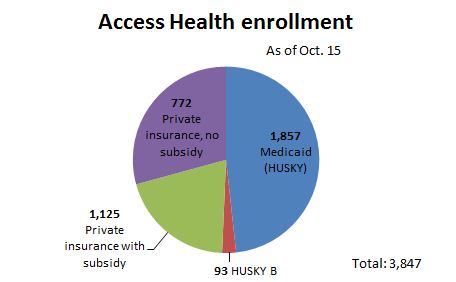
Of those who signed up so far, 48 percent — 1,857 — will receive Medicaid coverage. Another 93 are children who will receive subsidized coverage through the state’s HUSKY B program, a program for kids whose parents earn too much to qualify for Medicaid.
Among the 1,897 people who signed up for private coverage so far, 1,125 will receive federal subsidies to discount their premiums, and the other 772 won’t.
Peter Van Loon, the exchange’s chief operating officer, said that based on the phone calls he’s received, it appears that there’s been a lot of pent up demand from older residents who haven’t been able to get health care. “They have jumped on this in a big way,” he said.
Noting that a bar chart of enrollees by age showed more customers in the older age groups, Van Loon added, “We’ll have to keep track of this one because we want a nice bell curve, not just a slew to the right.”
Signing up young, healthy members is considered critical to exchanges’ success because those who don’t use many medical services will help balance out the cost of covering people who require more care. The health law prohibits insurers from shutting out people based on their medical histories, so it’s expected that many of the newly insured will be those who have not been able to buy coverage in the past because of their health.
Customers have a choice between coverage levels, referred to as bronze, silver and gold. Officials had expected about half to select the midlevel silver plans, with the more costly gold plans getting only about 12 percent of the business, Counihan said.
They were right about the silver plans, at least among the early shoppers. But so far, 26 percent of customers chose gold plans, which have higher premiums but require members to pay less when getting care. Counihan said Wednesday that that could indicate that the early buyers include a high concentration of people with pre-existing conditions, who might want plans that cover more medical costs. In addition, he said, because the federal health law limits how much rates can vary based on people’s ages, it’s possible that older customers are finding richer plans more affordable.
The people the exchange reports as having signed up for coverage are those who have completed applications and selected plans. The exchange still has to send their data to insurance companies, which will bill them for the premiums.
So far, two-thirds of the early customers have chosen plans offered by Anthem Blue Cross and Blue Shield. Another 31 percent selected plans sold by ConnectiCare Benefits. Only two percent signed up for plans offered by HealthyCT, a new nonprofit insurer created with federal funds made available through the federal health law.

Board members asked for data on the racial breakdown of those who signed up for coverage, but exchange officials say that information is not collected for all enrollees yet.
The agreement reached Wednesday to reopen the federal government included requirements that exchanges verify applicants’ eligibility for tax credits to discount premiums, which is based on income. Counihan noted that Connecticut already verifies eligibility.
“The practical impact on this to Connecticut is nil,” he said. But he added that it could have an effect on other states and the federally run exchanges.
Several board members praised the Access Health staff and contrasted Connecticut’s relatively smooth launch with that of the federally run exchanges.
Exchange leaders said there’s still much work to be done to get people to sign up for coverage.
Evelyn Barnum, CEO of the Community Health Center Association of Connecticut, told the board that community health center staff are working to sign up the uninsured, but need more support from the exchange.
Barnum asked that the health center workers doing outreach be recognized as much as the people from other organizations who are getting grants from Access Health to help people get covered.
“We’re trying to send the cavalry and we need you guys to help us and work with us at your end,” Barnum said.