 Enrollment is underway in the state’s health insurance exchange, one of the major pieces of the federal health reform law, and early numbers offer a chance to take stock of how things are going.
Enrollment is underway in the state’s health insurance exchange, one of the major pieces of the federal health reform law, and early numbers offer a chance to take stock of how things are going.
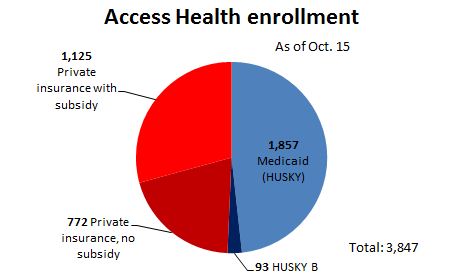
The exchange, called Access Health CT, sells private insurance plans to people who buy coverage on their own and to small businesses. It also enrolls people in the state’s Medicaid program, known as HUSKY, which is expanding Jan. 1 to cover more low-income adults who don’t have minor children.
How is it doing? Here’s a look at enrollment so far, what customers are buying, and how Access Health compares with exchanges in other states.
 Exchange activity so far
Exchange activity so far
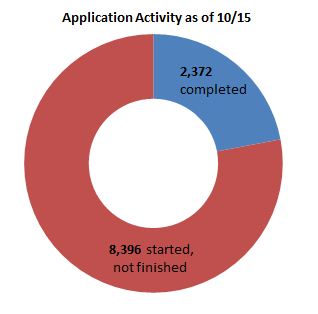
From its Oct. 1 opening through Oct. 15, Access Health enrolled 1,950 people in HUSKY and 1,897 people in private health plans. That’s more than officials had expected for the early days of the exchange. But it’s still a small fraction of the number of potential customers.
Connecticut has approximately 340,000 to 350,000 people without health insurance.
And the number of people in the market for health insurance is higher than that because the individual-market plans thousands of people currently have are being discontinued, requiring members to find new coverage for 2014.
Access Health’s open enrollment period runs through March 31. People looking for health insurance can also buy plans that aren’t sold on the exchange through insurers or brokers.
How does Connecticut compare to other states?
After some glitches in its early days, Connecticut’s exchange website has operated relatively smoothly. That’s in stark contrast to exchanges in some other states and, in particular, to those run by the federal government, which has faced enormous criticism for problems that made it difficult for people to sign up or browse for coverage.
As for enrollment activity, the amount of information released varies widely by state, as does the type of information being reported.
In Washington, for example, the state’s exchange has reported the number of people who signed up for insurance and paid their bills already (3,084) and the number of people who signed up for coverage but haven’t yet paid their bills, which are due in December (37,252). Washington has also reported how many people qualified for the state’s expanded Medicaid program (13,370) that starts in January, and how many applied and learned they qualify for Medicaid coverage now (8,495).
Kentucky, by contrast, reports enrollment as one figure, including people who have signed up for Medicaid and private insurance. And, unlike Washington, Kentucky counts someone as having enrolled in insurance regardless of whether the person has paid the first premium yet or not. (Connecticut’s enrollment figures also count people who have selected a plan but not paid the bill yet.)
There’s virtually no information available about the 34 states that have exchanges fully or partially run by the federal government. The federal government has not been forthcoming with information about how many people have been able to sign up.
Who are Connecticut’s early exchange customers?
So far, older people have been faster to sign up for coverage through Access Health than younger state residents.
Among people under 35, more are enrolling in Medicaid than in private insurance (known as “qualified health plans”). The reverse is true for people over 35.
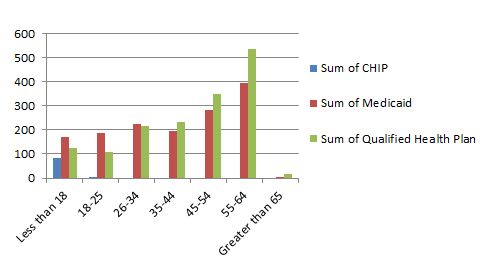
The age distribution of people who buy coverage through the exchange is considered a key indicator of the viability of the health plans. The premiums paid by younger and healthier people who use few medical services help balance out the cost of providing medical care to older and less healthy members. Because the health reform law prohibits insurers from denying coverage to people based on medical conditions, many of the new insurance customers are expected to be people with pre-existing conditions who have struggled to get coverage in the past. The extent to which younger, healthier people also buy insurance will help determine whether prices stay stable in future years or rise to account for the sicker population.
What are they buying?
 Access Health customers have a choice between three types of plans: Bronze, silver and gold. The bronze plans have the lowest premiums but require members to pay higher out-of-pocket costs — deductibles and coinsurance — when they get care. By contrast, the gold plans have the highest premiums but cover a larger share of medical costs, so members have lower deductibles and copayments.
Access Health customers have a choice between three types of plans: Bronze, silver and gold. The bronze plans have the lowest premiums but require members to pay higher out-of-pocket costs — deductibles and coinsurance — when they get care. By contrast, the gold plans have the highest premiums but cover a larger share of medical costs, so members have lower deductibles and copayments.
So far, just over half of the people signing up for private coverage have chosen the midlevel silver plans, which is what Access Health officials expected. But they were surprised that 26 percent have selected gold plans, more than twice what officials had anticipated. Twenty percent have signed up for the lower-cost bronze plans.
People under 30 have a fourth option too: Catastrophic plans that cost less but require paying more of the cost of care. Three percent of the exchange’s customers have chosen catastrophic plans.
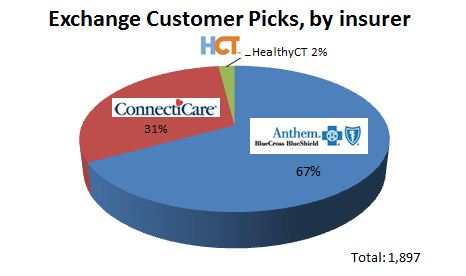 In addition, customers on the exchange’s individual market can choose between plans offered by three different insurers: Anthem Blue Cross and Blue Shield, ConnectiCare Benefits, and HealthyCT.
In addition, customers on the exchange’s individual market can choose between plans offered by three different insurers: Anthem Blue Cross and Blue Shield, ConnectiCare Benefits, and HealthyCT.
So far, the bulk of the business has gone to Anthem, the state’s largest insurer. HealthyCT, a new nonprofit plan created with federal funds made available as part of the health law, has the fewest members.


