Connecticut officials promoting Obamacare have touted the fact that more than 200,000 people signed up for health care coverage in the first six months the state’s new insurance marketplace was open.
But that doesn’t mean 200,000 more state residents have health care coverage.
For one thing, it’s not clear how many of those who signed up were previously uninsured.
And new data indicate that while Medicaid enrollment grew to a record level, the number of people covered didn’t increase nearly as much as the sign-up figures would indicate.
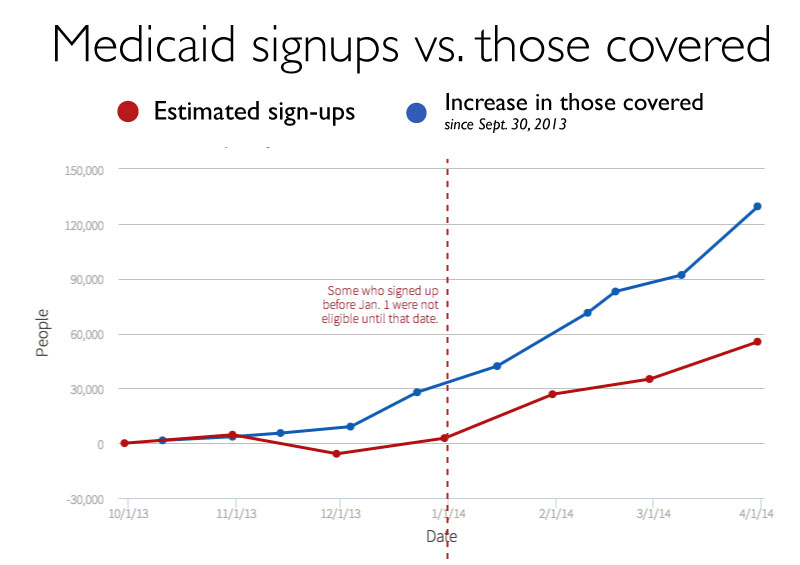
The bulk of the Connecticut residents who signed up for coverage as part of Obamacare qualified for Medicaid: 129,588 people, according to Access Health CT, the state’s exchange.
But that level of growth isn’t reflected in increased Medicaid coverage, according to figures from the state Department of Social Services. Instead, the department’s figures show that the number of people covered by Medicaid grew by 72,741 people — just over half the number that signed up.
The two numbers are not necessarily contradictory. The 129,588 figure Access Health has used represents people who signed up for Medicaid from Oct. 1 to March 31, while the DSS figure — 72,741 more enrollees as of the end of April — reflects program enrollment after accounting for people who dropped out of Medicaid.
But why such a large discrepancy?
People who track Medicaid enrollment said they aren’t sure, although they said there are possible explanations. One is that as people sign up for Medicaid, others are being cut off from the program — an explanation that underscores the importance of looking at not just how many people sign up, but how many are actually covered.
Another explanation is that there’s a lag in getting newly enrolled Medicaid clients’ information into the DSS eligibility system, which must happen before they show up on the department’s enrollment reports. While people in that situation are technically covered, many have said they’ve been unable to see doctors or get prescriptions filled because health care providers haven’t been able to verify that they’re enrolled.
Not everyone is convinced there is a gap. Access Health CEO Kevin Counihan said officials from his agency and DSS have not met to discuss the differing numbers, although his agency has tried. Until that happens, he said, he couldn’t confirm if any discrepancy exists. A DSS official said Wednesday that a meeting is scheduled for next week and that concerns about reconciling enrollment numbers between the two agencies “have been flagged for some time.”
One possible explanation: Churn
When some people are signing up for Medicaid, others are dropping out of the program.
This is known as “churn,” and it’s a constant in Medicaid (and other insurance programs). People drop out of Medicaid for various reasons: they’re no longer eligible, get other insurance, or don’t complete the paperwork needed to stay in the program.
In addition, some clients and advocates say, some people have been getting cut off Connecticut’s Medicaid program because of administrative glitches, even though they still qualify and sent in their renewal paperwork.
Because of churn, it’s unlikely that the number of people who sign up for Medicaid would ever match the growth of total enrollment in the program — that is, some gap is to be expected. But it’s not clear if churn would account for the entire discrepancy between the Access Health sign-ups and DSS enrollment numbers.
During the first six months of the Obamacare open enrollment period — from October 2013 through March 2014 — an average of 19,843 households were slated to be cut off from Medicaid each month, according to figures from DSS. The number of people that represents was probably higher because the majority of Medicaid clients are children and parents, with more than one person covered in the household. During that period, Medicaid covered more than 600,000 people.
The figures from DSS don’t identify why people were set to be cut off from the program, so it’s not clear how many no longer qualified for the program and how many would have inappropriately lost benefits.
And it’s not clear whether all of those people were actually cut off from the program.
Among Medicaid clients who recently tried to renew their coverage, about 14 percent have been found ineligible because their income is too high, Counihan said. The exchange, which now processes Medicaid renewals, directs people who earn too much for Medicaid to private insurance plans.
Churning is also expected among people in private insurance. Researchers at the Urban Institute projected in 2012 that nearly one in three people who get Medicaid or subsidized private insurance would churn off their coverage at least once in a year. Another recent study included predictions that more than 40 percent of adults who sign up for Medicaid or subsidized private insurance would experience a change in eligibility within one year.
Counihan said he expects that of the 80,018 people who have private insurance plans through the exchange, about 35 percent will not maintain their coverage for the full year. Already, about 7,000 people who signed up for private insurance through the exchange have dropped out (they’re not included in the 80,018 figure).
Another explanation: Delays on the DSS side
There’s a lag between when Access Health counts someone as enrolling in Medicaid and when DSS counts the person as being in the program. And that can be a difference of several weeks.
Access Health’s counts people as having signed up after the system deems them eligible for Medicaid and they indicate they want to enroll.
But those people won’t show up in DSS’ net enrollment reports until after their information is entered into the department’s eligibility management system. And that process takes time. Because the Access Health and DSS systems are not connected, Access Health must send information about the new enrollees as PDFs to a state contractor, where workers manually enter it into the DSS system.
DSS said in February that the data entry occurs within four days in roughly 73 percent of new Medicaid cases. In some cases, the data entry can take several weeks, spokesman David Dearborn said last week. Dearborn said the main reason for the delays is inconsistent quality of the enrollment PDFs that come from Access Health.
Could that explain the size of the gap in the two agencies’ numbers? It’s possible — but only if the lag is several weeks long for more than 50,000 people.
The 129,588 people Access Health reported as having signed up for Medicaid enrolled by March 31. The DSS enrollment figure that shows a growth of 72,741 members is from the end of April — a full month later. So unless the lag is several weeks long, it’s unlikely to explain the full gap between sign-ups and DSS’ number on people covered.
The delay in getting clients’ information into the DSS system has implications beyond data reporting. While people deemed eligible for Medicaid by the Access Health system receive a letter they can use as proof of coverage, many have said they’ve been unable to make medical appointments or get prescriptions filled because pharmacies and health care providers can’t verify that they have coverage until their information is entered into the DSS system.
DSS has notified providers that they should accept the letters as proof of coverage and, more recently, given them the option of calling to get a temporary ID number to use when submitting claims for new Medicaid clients.
Another difference: HUSKY B
One other way the Access Health and DSS numbers are not parallel: Access Health’s total includes sign ups for a public program known as HUSKY B, which covers children whose parents earn too much to qualify for Medicaid. DSS’ Medicaid figures don’t include that program.
But according to DSS, enrollment in HUSKY B dropped by 1,363 children — to 11,824 — during the first six months of the Obamacare open enrollment, so it’s unlikely to explain any gap in the two agencies’ figures.