The most familiar indicator of COVID-19’s inexorable nationwide spread —daily state and local case counts— may be on the way out.
Instead, public health officials are considering a shift from increasingly inaccurate case data to numbers they say better represent the effect of the disease on the community and the health care system: COVID-19 hospitalizations and deaths.
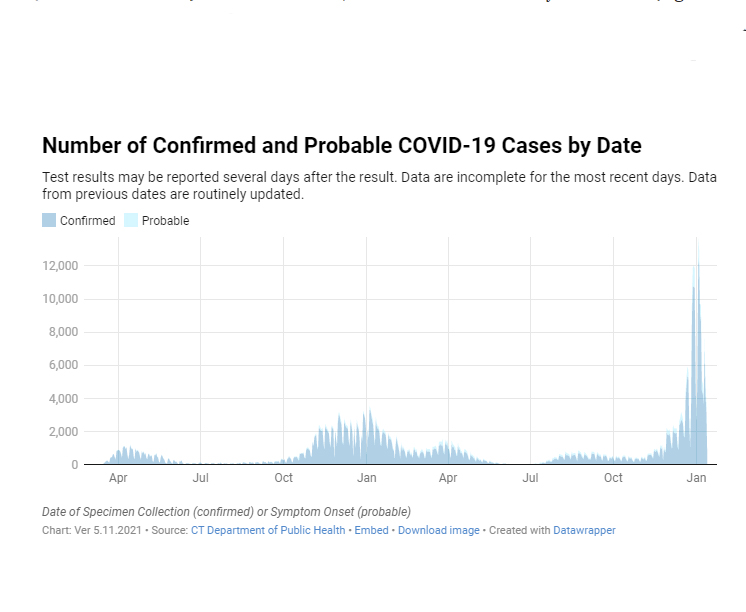
Omicron case counts are shattering all previous COVID-19 records. But the numbers don’t carry the same weight they used to. State and local health departments are preparing to explain that to the public and start reporting more meaningful data on the virus.
“The goal of public health data is to provide information to people so they can take actions to keep themselves safer and healthier,” said Meredith Allen, vice president for health security at the Association of State and Territorial Health Officials. “We’re getting to a point where a daily case count isn’t giving people that information.”
So far, Tennessee is the only state to scale back its COVID-19 case reporting since omicron hit. But experts expect other states to follow once the omicron surge subsides.
In addition, New York Democratic Gov. Kathy Hochul last week asked hospitals to start providing more meaningful COVID-19 data by specifying whether patients were admitted because of COVID-19 or entered the hospital for unrelated reasons and incidentally tested positive for the virus.
For now, daily case counts remain the primary gauge of omicron’s nationwide spread. But epidemiologists caution that the numbers should be relied on only as broad indicators of the velocity and direction of the disease’s transmission.
Because of testing shortages, unreported home tests and a high percentage of asymptomatic infections going undetected, daily case counts are vastly underreported, said Janet Hamilton, executive director at the Council of State and Territorial Epidemiologists. The true number of infections is some multiple of the reported cases, she said.
This week, the average daily reported case count was 781,000, more than three times the daily count of 250,000 at the peak of the delta surge a year ago. On Jan. 3, more than a million omicron cases were recorded.
But that doesn’t mean hospitalizations and deaths, which lag new cases by several weeks, will rise in equal proportion. Early data indicates that omicron infections are producing milder symptoms and fewer deaths than previous COVID-19 variants.
“We don’t want to keep telling people there’s X number of new infections out there without giving them an idea of how many of those cases will have serious outcomes,” Hamilton said.
Despite its lower hospitalization and death rate, omicron’s soaring infections are resulting in a surge in hospital visits, almost entirely among unvaccinated people, straining health care systems nationwide. And even though it’s proving less virulent than previous COVID-19 strains, omicron is expected to result in more deaths because of the sheer number of people infected.
Better barometers
Months into the pandemic, epidemiologists said COVID-19 ultimately would become endemic, infecting nearly everyone and remaining in the population indefinitely.
That endemic era may have started. As a result, many state health officials say they’re preparing to scale back the frequency of case count updates, possibly as soon as the current surge subsides, Allen said.
“That would allow public health agencies to focus on prevention efforts in high-risk populations such as long-term care facilities and work more closely with schools and vaccination clinics,” she said, “rather than put the time and energy into producing that daily number.”
Tennessee shifted from daily to weekly reporting of new COVID-19 cases Jan. 1, citing a need to focus on other public health priorities, including the expanding opioid overdose crisis.
Florida, Iowa and Nebraska moved to weekly counts last summer, as COVID-19 cases waned nationwide. Alaska, Kansas and Michigan publish case data three times a week.
For now, though, state and local COVID-19 policies, including school and business closures, travel restrictions, mask requirements and quarantine rules, largely hinge on daily numbers.
Since the pandemic began, the rise and fall of case counts has proven a reliable indicator of whether the virus is gaining ground, leveling out or retreating, said Dr. William Schaffner, professor of preventive medicine at the Vanderbilt University School of Medicine and adviser to the Centers for Disease Control and Prevention.
“We all know that the data is less precise than it was,” he said. “But we do get a good sense of the trends over time and geographically, particularly in a state that is long and thin like Tennessee. It allows us to look at what’s happening in Nashville versus Chattanooga, for example.”
The CDC official guidelines continue to recommend that state and local health departments publish daily COVID-19 case counts, he said. But in discussions with health officials, the agency is “giving states leeway to put more emphasis on hospitalizations and other data.”
Schaffner and other experts say the number of people hospitalized with COVID-19 may be a better indicator of the severity of the disease and its impact on communities and the health care system. Others argue that the number of patients in intensive care units would be a more meaningful measure.
Gray areas
As cases of omicron mushroom, it’s becoming increasingly likely that hospital patients will test positive for the virus upon admission or become infected while in the hospital, said Eili Klein, an epidemiologist and associate professor of emergency medicine at Johns Hopkins School of Medicine.
Even before omicron became dominant, studies showed that roughly half of patients admitted to hospitals with COVID-19 were there for other reasons. Still, their COVID-19 infections likely affected their health outcomes and the length of time they stayed in the hospital, Klein said, and it certainly meant the hospital had to expend additional resources to treat them.
It’s not easy to unspool COVID-19 hospitalization data, he said. “There’s a large gray area that’s difficult to determine in real time.”
Klein and other experts argue that use of intensive care is a better measure of the virus’ health burden.
“In Maryland, for example, hospitalizations are at an all-time high right now,” Klein said, “but use of intensive care is not.” Last year during the delta surge, hospitalizations in the state were much lower than they are now, but almost every patient was very sick.
“As we move forward, there needs to be some decisions about how we adjust our reporting,” Klein said. “Do we go to weekly reports, separate people admitted for COVID as opposed to those with COVID? It depends on how we plan to treat people who test positive but aren’t sick.
“Do we quarantine them? Maybe we stop doing that. We don’t quarantine people who have the flu.”
Testing shortages
From the beginning, testing shortages, inaccuracies and delays have plagued the nation’s response to COVID-19. As a result, many county and city health departments have never been able to publish daily case counts, said Adriane Casalotti, chief of public and government affairs at the National Association of County and City Health Officials.
In this omicron surge, she said, long lines at testing centers continue to stress city and county health departments, particularly as they field an avalanche of questions from the public about the CDC’s recent about-face on COVID-19 quarantines.
In December, the CDC announced that it was reducing its quarantine recommendations from 10 to five days. The American Medical Association and other experts called the weaker recommendations risky, suggesting that people get tested before ending quarantine.
With home tests still in short supply and people waiting hours to get tested at a public site, it’s a hard call for local health departments to suggest people get tested before they end quarantine, Casalotti said. On top of that, local health departments typically experience major public backlash when they try to implement stiffer COVID-19 restrictions than the CDC.
When will the testing shortage ease? President Joe Biden announced this week that insurance companies will be required to cover the cost of up to eight tests per person per month starting Jan. 15. But drugstores are still short of tests.
Mara Aspinall, a professor of biomedical diagnostics at Arizona State University, projects the nationwide supply of COVID-19 home tests will jump from 631 million tests this month to 732 million in February and 907 million in March. Since many consumers buy tests to have them on hand when needed, not all tests are used in the same month they’re purchased, she explained.
Since omicron hit the United States in December, Aspinall estimates Americans have been using an average of 4 million home tests per day, rising to 5 million per day last week as corporations distributed tests to employees coming back to in-person work. Whether that number stays the same, rises or falls depends on the spread of the virus, she said.
This story was originally published Jan. 14, 2022, by Pew Stateline.