Months after Stone Academy’s closure, more than 800 students across the state are waiting to hear the impact the nursing school’s abrupt end will have on the months or years they’ve spent studying to become licensed practical nurses.
A state-funded audit of their coursework and clinical hours is expected to determine a path forward in the coming months for the students, mostly women, who now realize they saw warning signs that the school was on shaky footing.
[RELATED: Stone Academy shut down. What does the future hold for its students?]
Many have said it feels like they’re grieving the death of a loved one — the loved one being their dream. Many have said they’ve been struggling mentally — stuck with uneasy feelings of uncertainty, depression and even suicidal thoughts. They all recall countless sacrifices they made for their programs — time away from family, thousands of miles traveled, leaving jobs and deteriorating relationships.
Many have asked themselves, “What do I have to show for it?”
Here are some of their stories.
Jarlinne Brooks, 33.
Jarlinne Brooks said her stomach had looked like a shark had taken a bite out of it as she recovered from a bad C-section birth in the early months of 2020.
Bed-bound at her grandmother’s house in New London, the television was always stuck on a telenovela or Telemundo. Every day she was taunted by a commercial that played so often that she took it as a sign.

It wasn’t a catchy jingle. It wasn’t a funny advertisement that sticks in your head. It was a Black woman speaking about being enrolled in one of Stone Academy’s programs. The words ‘Start your medical career,’ ‘Flexible class schedules,’ and ‘Job placement assistance’ floated on the bottom of the screen.
It had always been Brooks’ dream to become a nurse, but she had been too scared to pursue it, she said.
She has wanted to become a nurse since she was 5 years old. By the time she was 7, she was helping manage her grandmother’s unstable diabetes. She learned how to identify when someone’s blood sugar is too low and how to administer insulin.
A few years after high school she decided to pursue a career in health care. It began with medical billing and coding before she became a certified nursing assistant. From there, life took her through a whirlwind of jobs: in children’s behavioral health, with developmentally disabled adults and even career counseling for a college in Massachusetts.
But with two children under the age of 2, finishing up healing from an open wound and unemployed, Brooks thought it was the time to take the leap, so she did.
“Becoming an LPN will help with financial stability, it will offer myself and my babies a sturdy foundation to lean on and help keep us afloat,” Brooks wrote on her application, dated June 22, 2020. “I could actually start to save for them so they can one day go to college and consider paths they’d like to go on. Most importantly, I’d be able to work toward getting them our own place.”
She enrolled in a 15-month program, but, almost three years later, Brooks still doesn’t have any credentials.
“This is embarrassing. I’ve been in this for three years that I have nothing to show for. My grandmother’s not alive [anymore] to see me become a nurse,” Brooks said, crying. “This is so disgusting. It makes me want to throw up every time I think of everything that I dealt with at this school.”
In the beginning of her program, she noticed red flags, like a clinical director resigning the day after she met her in the beginning of a semester. Some days, her clinicals consisted of taking temperatures for several hours.
According to the state’s nursing education programs and licensure requirements, during clinicals, practical nursing students are supposed to spend at least 750 hours collecting data and “perform[ing] therapeutic nursing interventions.” This traditionally includes things like helping administer medicines, taking vitals, charting medical records, inserting and caring for urinary catheters and changing bandages.
In addition to only performing temperature checks, some days Brooks’ clinicals were canceled with no notice or she was told to write her name on a piece of paper and go home, she said.
“They didn’t care about us, and you knew it was a failing system,” Brooks said, adding that she tried to transfer out of the program within two months but didn’t because she felt she would take a huge financial hit due to the school’s refund and transfer policies.
“I’m literally asking to become a nurse. That shouldn’t be hard. I’m asking to become someone, something — a nurse — and I’m asking for the educators to help me get there, that is it,” Brooks said.
Beyond program delays, Brooks failed her exit exam twice, something she says was a product of the school setting her up for failure.
“I will say skill set wise, I have a good amount of skills. But let’s say, knowledgeably, I don’t believe I was ready,” Brooks said. “I wasn’t prepared appropriately [by the school] as I should have been.”
Brooks said she often had to teach herself the material.
For example, during COVID-19, instead of having online classes, teachers would only hop on the Zoom meeting for a few minutes to to assign homework and tell the students what chapters to read, then they were tested the following week, Brooks said.
Brooks also felt the institution preyed on young women of color who are trying to break generational curses but instead leaves them trapped with broken self-esteem.
“It was a misleading advertisement to attract individuals like me, who may have not had the best upbringing, and who is currently a single parent, and who’s struggling to make ends meet while I work and take care of my kids,” Brooks said. “So they post these types of schooling to attract us. Yeah, I was attracted because, you know, ‘Fast, fast, fast – 15 to 18 months for your LPN.’ ‘OK, I’m gonna do it.’”
Throughout her time at Stone, Brooks lost her grandmother, who was her sole motivation in becoming a nurse. Determined to still make her proud, Brooks began leaving her infant son with her grandfather three times a week and her daughter with her mother while she was in classes. She said she put over 60,000 miles on her car by traveling from New London to East Hartford.
“So much wasted time. So much wasted time. So much wasted time,” Brooks said.
She was in Stone’s remedial program at the time of its shutdown and preparing to take her exit exam again. Since the school’s closure, Brooks said she’s been stuck in a “mental fog,” that’s “taken a toll on me mentally, physically and emotionally.”
“But, I know I’m going to become a nurse,” Brooks said.
She hopes that however she gets her LPN or RN certification in the future, that she’ll be able to work at a correctional facility or psych ward.
Patty Bapst, 50.

Many people leave their jobs behind.
Patty Bapst was tired of jobs leaving her behind.
She had moved from Buffalo, N.Y., to Connecticut because of a romantic relationship. For the next 18 years, she worked in a factory making industrial pipe fitting covers. With five days’ warning, the company had decided to shut down. She then spent six years at Talbots, first as a saleswoman before working her way up into a management position, but the impact of COVID-19 killed the store.
“I wanted something that wasn’t going to close. I mean, being an industrial penetrator, which was the job title at the first job, that’s not a highly sought skill,” Bapst said. “I just wanted somewhere where I could be stable and do something that I enjoy and help people. … So I decided to go into a nursing program. … There’s always a need for nurses.”
Bapst grew up in a family full of veterinarians, so the medical field was in her blood already, she said. She had taken certified nursing assistant classes in New York several years ago and had been putting that education to use after her sister moved in with her in 2012 because of serious health issues.
After a stroke left Bapst’s sister unable to go up and down stairs, and suffering from a condition called “alien hand syndrome,” she was later moved to a nursing home. Bapst said she couldn’t let go, so she decided to work there part-time to still care for her sister.
All of those events led to an internet search for LPN programs. Stone Academy’s 22-month program was enticing. It was also the closest program to her home in Norwich.
Bapst enrolled in June 2021.
“That first semester was really good. I actually felt like we were getting somewhere, and then it started going downhill from there,” Bapst said.
Teachers were in constant rotation — Bapst recalled a teacher quitting mid-test. Attendance stopped being taken. Her cohort fell behind in clinicals because of lack of staffing and space. Bapst’s graduation date was set for May 2023, but she was already expecting it to be delayed for months because of issues with clinical hours.
On top of stress from school, Bapst’s close friend Conrad Jurgensen, whom she considers an adopted father-in-law, was diagnosed with squamous cell carcinoma, a type of skin cancer, in late 2022.
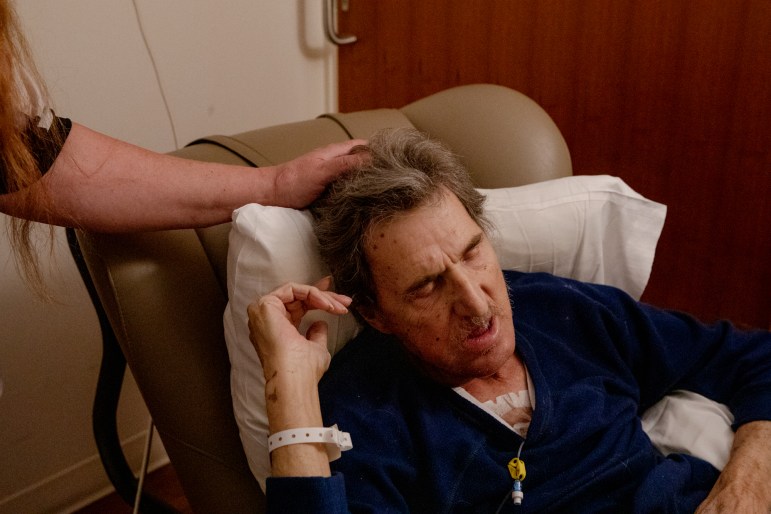
He underwent a surgery to remove his jaw, then was in chemotherapy and radiation treatment. One day while Bapst was leaving the hospital, she heard nurses talking about Stone Academy closure rumors.
She decided to stop by campus and ask what was going on. The staff told her they had no idea.
Within days, the school had sent an email saying it was shutting its doors. A text group chat among her clinical group began spamming with questions and expletives.
“It’s like a death almost — no, it is the death of a dream,” Bapst said. “I just was sitting there shaking my head. That was all I could do. I was just like, ‘I don’t know what to do.’”
In the last few weeks since the closure, Bapst said she has had to compartmentalize to not think about the uncertainty with school.
“I just been doing day to day. I don’t have the mental capacity to deal with this and deal with my job where I’m dealing with people with Parkinson’s and people with dementia and people with large injuries,” Bapst said. “… I’m hanging from a string on the end of a rope.”
A small piece of her feels like the closure may have been a blessing in disguise as she continues to take care of Jurgensen. But the other part of her knows, if the state comes back and says she has to restart her education, it’s the end of her nursing journey.
“I don’t even know that I want to say that I went to school at Stone, because it’s so bad,” Bapst said. “It’s wasted time, broken dreams, stolen futures. They’ve wasted our time and destroyed my dreams. And I don’t think I’m going to be able to go into the medical field if it goes this way.”
Ashley Garcia, 36, and Christina Carlson, 37.
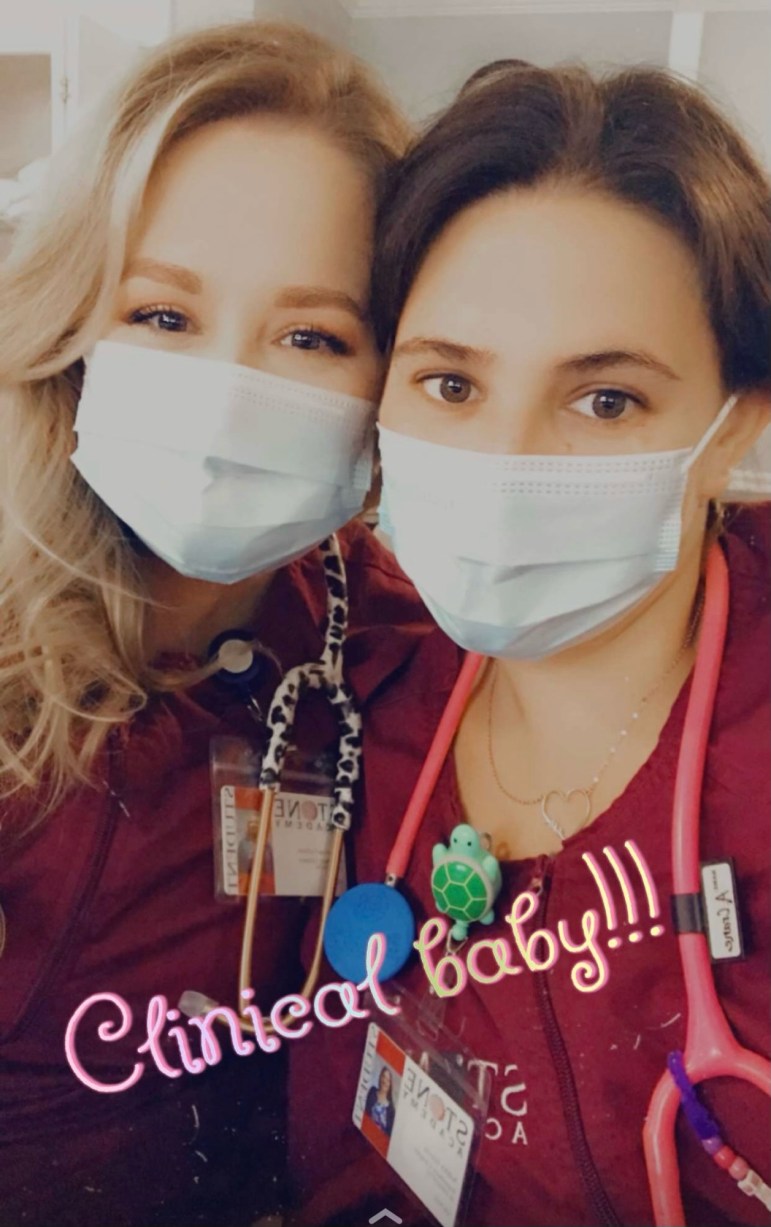
Anytime Ashley Garcia puts her mind to something, she says she has to drag her best friend, Christina Carlson, along for the ride.
That’s how the best friends went from working together at a Subway in their early 20s to obtaining their CNA certification before they went separate ways for their careers. The two reconnected when they began working at the same hospital in northwestern Connecticut and have been inseparable since.
Garcia had always wanted to be a nurse. She went to a local college to pursue an RN degree. She finished her prerequisites then applied to the competitive program three times.
When she was denied her third time, she hopped into Carlson’s car and cried.
Afterwards, she grabbed her best friend and told her, “Get your checkbook out, we’re going to become LPNs instead then.”
Carlson’s path was a little different. She didn’t know what she wanted to do or who she wanted to become, but her best friend became her “inspiration,” “booster” and “positivity,” she said.
“She always had the belief in me whereas I don’t,” Carlson said. “I’ve always had in my mind that I’d love to be a nurse, but I make excuses. ‘I’m not smart enough. I can’t do this. I can’t do that.’ [So the day she didn’t get in], we researched LPN programs, and I came across Stone Academy.”
The pair decided to drive over to Stone Academy’s Waterbury campus, but their GPS was accidentally set for Porter and Chester. They laugh about it now because it feels like it was a sign.
They enrolled in Stone Academy in June 2019. What was supposed to be a 22-month program has been ongoing for nearly four years.
They failed their initial exit exams before being put into a 16-month remediation program. They said only two of 24 students passed their cohort’s exit exam.
The best friends were supposed to graduate this July, but that seemed unlikely too. They were waiting for their clinical placements for several months and didn’t believe they’d finish in time with enough hours.
“I’ve got three and a half years, and I have nothing to show for it, and now I feel so defeated. I’m not saying 37 is old, but I don’t know what is going to happen. Nobody has the answers for us,” Carlson said. “I don’t want to be in my 40s going back to school. It already is hard with everyday life. I put my life on hold and I put having kids on hold because I knew I couldn’t be pregnant and be in school. And now I’m at the point where I’m at the age where I don’t even know if I can have kids because I’ve waited too long.”
For Garcia, the delays meant she had her second child while she was enrolled at the nursing school.
“I have a husband, I have two boys. That’s my responsibility as the mother, and I was supposed to be done with school and it was going to be no worries having another baby,” Garcia said, adding that she was hopeful her second child wouldn’t have to undergo the same sacrifices her first son had.
“I would barely see my older son. He’s going to be 7 next month. I literally would get him off of the bus and leave, and when I got home, he was sleeping,” Garcia said. “I missed out on all that time that I could spend with him going for a walk — anything — playing a game, reading a book, whatever. … I would leave at four o’clock in the afternoon. I didn’t get back until almost 11 o’clock at night.”
The pair said they began noticing the quality of the program decline during COVID-19. For an eight-week class, they had six different instructors. Then, they no longer had to sign in for attendance. Test scores were inaccurate. The school even raised the passing grade for the exit exam, so the score that would’ve allowed the friends to graduate was invalid and too low by the time the change was made.
Garcia and Carlson didn’t have class the night Stone Academy closed. Carlson had seen “school closure” on a news channel but thought it was because of the weather.
“It didn’t pertain to us because we didn’t attend school on Tuesdays, and I’m like, ‘Oh, that’s bizarre,’ but I continued on. I’m about to make some coffee, get ready to sit down and study and then everything blew up,” Carlson said.
“Yeah, it was an afternoon. It was 3:30, I had just woken up from a nap [with my newborn],” Garcia said. “I was going to get my [6-year-old] son from school, and I just happened to open up my email and I saw a letter from Stone Academy. I opened it real quick, and they said that they were going to be closing and I just was ‘Is this a bad dream? Like, am I not awake?’”
Since the school’s closure, the friends have stayed busy through their work at Charlotte Hungerford Hospital, but it’s hard.
“Every day I go to work and everyone’s asking me about this, and I’m kind of at the point where I wish I could record myself and just push play because I have to repeat myself every day, and it gets emotional,” Carlson said. “People commend me for being composed and holding myself together, but at the same time, I’m not. I don’t know what to feel anymore. I’ve already cried. I’ve already got angry. It’s kind of like no more emotion.”
After the audit comes back, the best friends said they’re more than willing to redo their clinical hours, if needed.
“I don’t know, somewhere deep inside there’s like a little piece of me that is like ‘You’re gonna make it. You’re gonna be OK. Everything’s gonna work out. What’s meant to be is meant to be,’” Garcia said.
However, if their programs need to be restarted, they’re split.
“I’m at the point where I just try not to be negative, but I just feel like my dream has been taken away from me,” Carlson said. “I only speak for myself, but I cannot go through all that heartache, sweat, tears, sleepless hours of studying again for something I’ve already completed.”
As Carlson spoke, Garcia shook her head.
“I told her there’s no such thing as giving up,” Garcia said.
“I didn’t give up,” Carlson said. “My dream was taken from me. I didn’t give up.”
Susan Anthony, 32.

When Susan Anthony goes in to work at Hartford Hospital, sometimes she sees nursing students, and it brings tears to her eyes.
“That should be me,” she says.
It took a week to call her mom and tell her she was no longer a student at Stone Academy because the school had shut down eight months into her 22-month program.
At first, she just got a headache. It was a surreal feeling when she got the email saying the school would not be continuing classes. The feeling reminded her of when Michael Jackson died, Anthony said with a small laugh.
“That’s just how sudden it was. It didn’t feel real,” Anthony said.
Then, when the news finally hit her, she couldn’t stop crying. Some days, when she would go in to work, she would break down in tears in her coworkers’ arms. She didn’t know how to spend her free time, which was usually occupied by reading her text book, watching nursing videos on YouTube or studying.
Two months later, she still has days where she wants to go into the back room and cry. She struggled with suicidal thoughts for a few weeks.
“It felt like I was grieving. I was this close to calling the resource counselors that they have for employees at work just to see if I can have someone to talk to,” Anthony said. “I felt like I was going to need counseling after this, like emotional counseling. I needed someone. I needed constant reassurance that I was going to be OK. There were times where I went to work and I’d be very angry. I’d be very sad. I’d be crying.”
It felt like “cruel timing,” she said.
Anthony, who is originally from New York City, previously worked as a medical assistant at a hospital in Brooklyn. She had been accepted into a nursing internship, then the hospital shut down and filed for bankruptcy.
“It just feels like a big slap in the face. It feels like history repeating itself 10 years later, it just broke my heart,” Anthony said. “I don’t like being a pessimist. I don’t like being a negative thinker. It’s just more of, ‘is nursing really right for me?’ All of this hitting me like this.”
When she moved to Hartford a few years ago, she enrolled at Goodwin University in East Hartford for its registered nursing program. She transferred out of the school after feeling “misled” and said an academic advisor was trying to make her take additional classes and prerequisites she already completed. She needed another school with flexibility and applied to three other Connecticut nursing programs including at Capital Community College and Stone Academy. She was waitlisted at Capital, and her eagerness got the better of her.
“I was so desperate to start because I was so frustrated about being waitlisted in the RN programs and stuff. I was very, very desperate, and desperate times call for desperate measures,” Anthony said. “I just wanted to pursue my career in nursing regardless of what route I took to get there. I just wanted to get it done.”
She never had suspicions about the academics at Stone Academy when she was enrolled. She went through her program thinking, “Whatever. Don’t question anything. Just do the damn thing. Go through it,” she said.
The waiting game to see if any of those eight months counted toward completing her certification is the worst part now.
Her motivation through the program was the excitement to transition from being a personal care assistant to an actual nurse — something she’s wanted since she was young.
“I just feel like I enjoy making people feel better, because it makes me feel better knowing that I go home and I feel good about myself knowing that I’ve made a difference in someone’s life,” Anthony said. “And I was trying to see that’s why I wanted to do nursing my whole life — to see if I can try to do that more of an absolute level.”
Now, she has to depend on affirmations, prayer and staying busy to get by the next few months as she waits for answers.
“All the encouragement that I’ve been receiving, gave me a lot of strength. … But, progress is not perfection,” Anthony said. “I’m not going to lie. I’m not OK. I was always told if you’re not OK, yell it out, and I’m not OK. It’ll get to someone’s ear. Something will be done about it. … [But right now,] a lot of us aren’t OK.”






