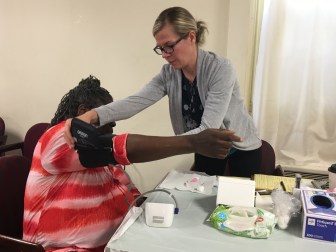
Bridgeport — Clara knew something was wrong with her health, but because she can’t speak English and doesn’t have a doctor, she didn’t know where to turn for help.
It wasn’t until she found her way to the basement of a church at an event hosted Wednesday by the Greater Bridgeport Primary Care Action Group that Clara – who asked that her last name not be used – finally found help. And it came not by way of a traditional doctor, but by a community health worker.
“She is an immigrant and doesn’t have health insurance so I need to help her get signed up for Americares,” said Millie Seguinot, a community health worker (CHW) for the Area Health Education Centers of Southwestern Connecticut. Seguinot, who was working the Bridgeport event, determined that Clara has high cholesterol, is most likely pre-diabetic, and needs to see a physician.
Clara, who moved to Bridgeport from Venezuela a few months ago, was by no means the only person who found help at the Wednesday morning event in Bridgeport.
More than a dozen individuals were having their blood pressure checked, learning about blood sugar testing, and stopping by the Community Health Worker (CHW) table at the back to connect with a doctor, learn about dozens of free assistance programs and, best of all, speak to someone in their own language.
The goal of these events is “to help people to stop using the emergency department as a primary care office and prevent health crisis that are avoidable,” said Gina Smith, a health educator from Bridgeport Hospital,

Bringing healthcare directly to the community also helps individuals understand how to interpret lab tests and medical exam results, and addresses the basic needs that may prevent them from being compliant.
Community health workers across the state help to bridge the gap between the health care system and communities, said Tiffany Donelson, vice president of programs at Connecticut Health Foundation. With the growing push toward value-based payment methods, accountability for outcomes, and the focus on social determinants of health, CHWs have proved increasingly important in creating effective care in lower income communities.
“They are the interface between what the patient needs and what is happening clinically,” Donelson added.
In addition to addressing language barriers, CHWs help solve access problems related to transportation, finances, shelter, and application procedures.
Despite their value to the health care system and the underserved communities they reach, however, there is still no sustainable funding for the majority of the workforce because their services are not covered by insurance.
“The grants run out and whatever you have done is cut off,” said Fataw Mahams, a CHW working with Seguinot on Wednesday. “If you have scheduled appointments with patients and the grant ends, that’s it. But sometimes we still do it even without getting paid, we care so much. We still want to help.”
This instability is nothing new.
“They (CHWs) have [mostly] been paid through grants or soft money,” said Meredith Ferraro, the executive director of area health education centers. “People always said ‘I don’t know how long I’m going to have this job’ because they didn’t know when the money would go away.”
And that’s where the push for certification comes in.
“The idea for certification is to recognize the CHW workforce as a viable workforce that actually connects communities to resources and care,” Ferraro said.
The hope is that if the CHW workforce is professionalized through certification, insurance companies will begin paying for their work, creating a more sustainable form of funding.
“We hope certification gets us closer to a situation where payers are comfortable with the role of a community health worker,” Donelson said. “It will give payers and employers confidence in the workforce. They will truly understand that there are standards around education and scope of practice for CHWs so that they are employed, utilized and funded.”

A recommendation for certifying community health workers was recently developed by the State Innovation Model (SIM) committee. The report recommends two pathways to certification through the Department of Public Health, including one with standardized education and training and one that takes into account previous work experience.
“We want the certification to mean something while not being too burdensome,” said Jenna Lupi, a care delivery reform specialist for the Office of Health Strategy, who presented the recommendations at a SIM meeting this month.
The report has yet to be sent to legislators, but Sen. Terry Gerratana D-New Britain, a co-chair of the Public Health Committee, said she is interested in anything that may help to reduce health disparities and increase access to healthcare.
“Sometimes we find that people will just go to their nearest emergency room for health care when they would get better services in a different setting,” Gerrantana said. “To have community health workers connect individuals with resources and provide outreach throughout the community helps everyone.”
Gerrantana said she may bring the issue up in the committee this session, depending on the priorities of the new administration.
“I think there are a lot of players who want to see health equity in the state and I think moving this workforce forward to try and minimize the health disparities will help to get there,” Lupi said. “We hope it passes this session, but I know anything with a fiscal note is going to be a challenge.”



