Last year, U.S. Sen. Richard Blumenthal (D-CT) provided an important service to patients struggling with serious illnesses. He chaired a Senate hearing on the role that pharmacy benefit managers, or PBMs, play in the price and accessibility of critically needed medicines.
In that hearing, Sen. Blumenthal pointed out that the largest PBMs – who hold the power over medicine availability for millions of Americans – were excluding hundreds of drugs from their formularies and, therefore, making them inaccessible to patients.

Since that hearing, the PBM stranglehold on our health and well-being has only tightened. Out-of-pocket drug costs are unaffordable for far too many, and the system has been structured to force patients to use medicines that are best for the PBMs’ financial bottom line even if they are not what our physicians have determined are best for treating our conditions.
It’s time for Congress to translate its investigations into concrete action when it comes to the practices of these corporate middlemen.
This is a matter of great concern and urgency for those with serious, complex diseases like HIV/AIDS and cancer. Our body chemistries are not identical and certain medicines have greater effectiveness with some patients than others or, conversely, may cause harmful side effects for some. It is critical that when medical professionals determine the best drug or combination of drugs to treat a severe illness, those treatments are affordable and accessible.
The PBMs were originally charged with making that happen. They were the negotiators who worked with multiple health insurers and public plans like state Medicaid programs, using accumulated purchasing power to leverage favorable prices from the drug manufacturers. Over time, though, the industry has undergone significant consolidation and now only three multi-billion-dollar companies control 80% of the prescribing market. Unfortunately, they use that power for their own interests rather than those of patients and consumers.
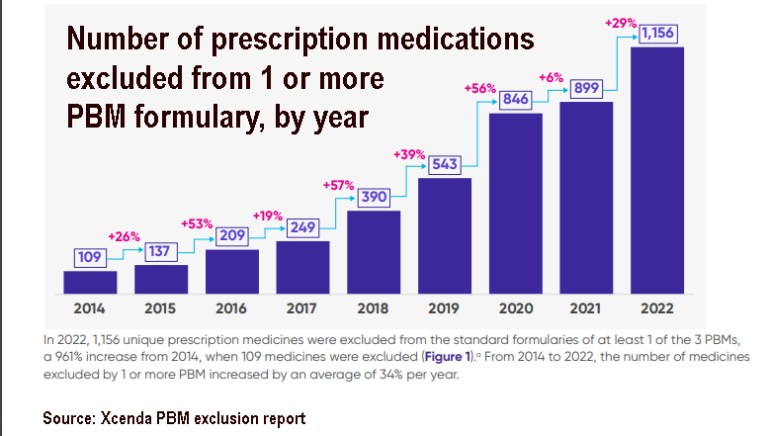
In 2014, only 109 prescription medications were excluded from one or more PBM formulary. By 2022, that number had escalated to 1,156. The number of excluded drugs has gone up every single year. These are medicines that the PBMs have determined will not receive insurance coverage, forcing patients to pay full list price or use the PBM-preferred medications. It’s safe to say that very few people can afford a specialty drug’s list price.
Why is this happening? One reason is because the PBMs have created a reimbursement structure in which they make more profit, through administrative fees and rebate deals, when a drug’s list price is higher. So, the medicines that don’t generate favorable revenues for the middlemen have a greater likelihood of being left off formularies, constricting the therapeutic options available to patients. This anti-consumer environment has, thus far, evaded solutions because the PBM business practices are both highly complex and incredibly opaque.
It’s essential for Congress to act and even the scales that have tilted too far in favor of corporate interests. Bipartisan legislation introduced by Sens. Maria Cantwell (D-WA) and Chuck Grassley (R-IA) would force these companies to make their actions more transparent and would bring an end to deceptive and harmful pricing practices. This legislation is a good start, even if more needs to be done to ensure that the discounts and rebates PBMs are negotiating with drug manufacturers are shared with consumers and not just transformed into profits.
There are people in our state today who are suffering from serious illness and are unable to get the medicines they need. This is simply incomprehensible in our society. Sen. Blumenthal and others have helped narrow the focus on where the problems lie with drug access and affordability. Now it’s time to do something about it.
John Merz is CEO of Advancing CT Together/Hartford.



