Chances are, you or someone you know has been affected by colon cancer. According to the National Cancer Institute, Connecticut had nearly 61 cases of colon cancer per 100,000 residents in the early 2000s.
In 2020, the incidence decreased by half. You may ask, why is that? The answer is: screening, early detection and early intervention.
In September of 2012, a federal law in the Affordable Care Act was passed mandating health plans to cover colorectal cancer screening according to national recommendations of the United States Preventive Services Task Force. Undoubtedly, social determinants of health have a tremendous impact on screening, early detection and early intervention despite this mandate.
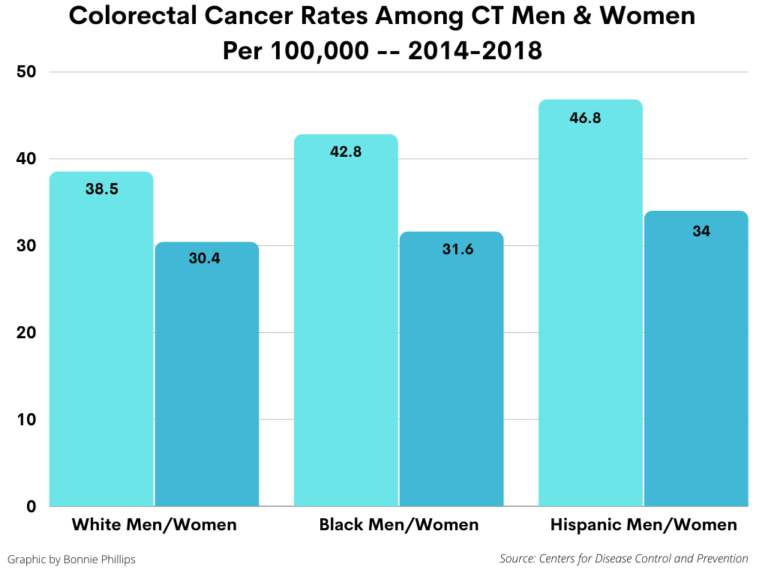
Statistics from the National Institute of Health show that prior to the COVID-19 pandemic, Black Non-Hispanic people of color in Connecticut had no decline in the incidence of colorectal cancer while all other races and ethnicities had decreased incidences of colon cancer. Individuals of Black race are disproportionately affected by colorectal cancer with higher rates of death according to the Centers for Disease Control and Prevention, The American Cancer Society and the United States Preventive Services Task Force. National research has shown that the COVID-19 pandemic has had a worsening impact on this statistic due to delays in screening.
Methods of screening include stool-based at-home tests that are mailed into the appropriate agency or direct visualization like a colonoscopy. While stool-based screening provides greater access and less burden, if it is positive, a diagnostic colonoscopy is recommended. This diagnostic colonoscopy poses burdens of finances, preparation, and transportation.
To address the financial burden, the Centers for Disease Control and Prevention has provided grants for Connecticut residents to have this diagnostic colonoscopy at no cost for individuals meeting the eligibility criteria outlined on Connecticut Colorectal Cancer Control Program (CCRCP) website. While this program can close the gap in obtaining diagnostic testing amongst disproportionately affected populations, it still has its pitfalls.
Barriers to obtaining the diagnostic colonoscopy through this program include transportation and cost of preparation. As a registered nurse, I know that patients have opted out of this potentially life-saving study due to lack of transportation and cost of the preparation materials. The CCRP does not outline additional support for medical transportation or vouchers to obtain the necessary colonoscopy preparation materials.

Transportation may be the biggest barrier given that the program partners with only five facilities throughout the state. Veyo, Medicare and Medicaid’s non-emergency medical transportation company, reported 79% of members needing transportation outside the permitted 10–20-mile range in recent years. Given this, it seems almost impossible for majority of Connecticut residents to have non-emergency medical transportation covered through insurance to travel to one of the participating facilities. These disadvantages to a potentially life-saving diagnostic study should not exist within CCRP when it seeks to close the gap in care delivery for disproportionately affected communities.
If you or someone you know meets CCRP eligibility, act now! We need more support for our disadvantaged community members. I urge you to speak with your local legislators on how the CCRP can be more inclusive in its offerings of diagnostic colonoscopies after a positive stool-based screening. Advocate for exceptions in mileage restrictions for medical transportation coverage at no cost to the consumer, should it be needed, and vouchers for preparation materials for the diagnostic colonoscopy.
Contact your local legislators asking for enhancements to CCRP for increased availability and accessibility to diagnostic colonoscopies in accordance with recommendations of national prevention organizations. You can do this through the Connecticut General Assembly website. Remember, early detection and early intervention can decrease your risk for detrimental outcomes.
Speak with your primary care provider on which screening method is best for you. Stool-based screenings are readily available and covered by most insurances. According to the National Institute of Health, the COVID-19 pandemic delayed in-person colorectal cancer screening which can lead to an increase in colorectal cancer diagnosis within the following decade. Don’t delay your screening. Let’s close the gap on barriers to screening for disproportionately affected communities and advocate for those who may not be able to advocate for themselves.
What can you do today? Reduce the risk for colon cancer and optimize your health with a nutritious diet high in non-starchy vegetables, fruits, whole grains and low in red and processed meats. Get regular physical exercise and maintain a healthy weight. Abstain from tobacco and alcohol to further reduce your risk for cancer. If you have been diagnosed with health conditions, work with your primary care provider on how you can ensure they are well managed. Make healthy habits daily and stay up to date on your routine health screenings.
Talk to your local government representatives about small changes that can have a large impact on you and your local neighbors’ health.
Arianna Burkard is a Registered Nurse and Family Nurse Practitioner student at the University of Connecticut.