The rollout of the federal health law in Connecticut has been smoother than in many parts of the country, but it hasn’t been without hiccups. The latest one: finding providers who take the new coverage.
Some of the more than 60,000 people who have bought private insurance plans through the state’s exchange, Access Health CT, have had trouble navigating their plans’ networks of covered health care providers.
“There remains confusion, I think, about the networks,” Access Health CEO Kevin Counihan said. “Everybody’s sensitive to it. It’s clearly a big member issue.”
In some cases, people who called to check if a provider would take their insurance arrived at the appointment only to find out their coverage wouldn’t be accepted, state Healthcare Advocate Victoria Veltri said.
Some of the confusion isn’t unique to the exchange plans. But the creation of a new set of insurance policies and the shift of thousands of people into new coverage all at once has added a new set of challenges.
“The fact that we have such a high volume of people searching for providers is kind of shining a spotlight on an issue that we need to remedy,” Veltri said.
What’s the problem?
There are several reasons people are having trouble finding doctors who take their insurance. But perhaps the biggest source of confusion is that the plans sold on the exchange by Anthem Blue Cross and Blue Shield and ConnectiCare use different networks of health care providers than the plans each company sells outside the exchange.
That means it’s not enough to call a doctor’s office and ask if he or she takes Anthem or ConnectiCare. Instead, people with coverage purchased on the exchange must ask if a provider takes the Anthem or ConnectiCare plans sold on the exchange — something not all would-be patients have done.
Dr. Michael Krinsky, a neurologist, said sometimes patients call and say they have a certain insurer’s plan, but don’t say that it’s the coverage purchased on the exchange. “It becomes a puzzle for the front office staff to unravel on the telephone,” he said.
And in some cases, doctors don’t know whether they accept exchange plans. Many don’t negotiate directly with insurance companies. Instead, they belong to larger organizations that handle contracting. Krinsky, for example, had to check with the physician-hospital organization he belongs to to see what exchange plans it had contracted with.
“Your doctor may think they take Anthem and ConnectiCare, which they do, but these exchange networks are completely new and different, and they are smaller than networks already established,” said Tim Tracy, a Fairfield insurance broker and president of the Connecticut Chapter of the National Association of Health Underwriters. “You’re definitely seeing some disruption there.”
The third insurer selling plans on the individual exchange, HealthyCT, has the same network for all of its plans, whether sold on the exchange or not. But 97 percent of the exchange’s private insurance customers are covered by Anthem or ConnectiCare.
Another source of confusion: Network lists
The exchange relied on the insurers to provide online directories of their networks for potential customers to examine.
But when the exchange opened for business in October, some customers had trouble searching Anthem’s directory because the company’s website didn’t make clear which network lists applied to the exchange plans (the exchange plans were listed as “Pathway X”).
The company revised its list labels in November to note which networks are for exchange plans, and now people using the Access Health website who want to see the network associated with a particular Anthem plan are linked directly to the specific network.
In some cases, Veltri said, people have gotten medical care from a certain provider because they got information from a network directory that turned out to be inaccurate. In those cases, her office has asked the person’s insurer to cover the visit, and the carriers have been cooperative, she said.
“Anytime there’s going to be a new thing like this, I think there’s going to be issues around lists,” she said. “My immediate concern is to make sure the lists are accurate and to the degree people have purchased based on inaccuracies in lists, we need to make sure those people, if they complain, are informed of their options, including changing plans.”
The exchange networks are smaller than the other networks
It’s not just that the exchange networks in the largest plans are different. They also cover fewer providers.
Connecticut’s exchange has stricter network standards than many other states, where exchange plans have a small fraction of the number of providers as other plans. Access Health requires that plans it sells have networks that are substantially equal to those the carrier sells outside the exchange.
That standard only applies to one carrier on the individual exchange, however, because ConnectiCare’s exchange plans are part of a separate entity, ConnectiCare Benefits Inc., and HealthyCT has only one network.
Exchange officials have raised questions about whether Anthem’s exchange meets its benchmark. Anthem spokeswoman Sarah Yeager said the company’s exchange plans meet the standard, and she noted that Anthem’s exchange network is the broadest of any carrier participating with Access Health.
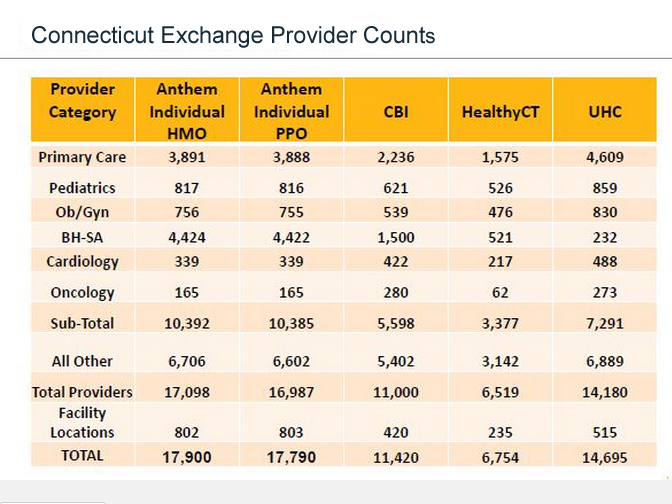
Yeager said Anthem has more than 22,000 providers in its off-exchange networks. The company’s individual exchange plans cover about 20,000 providers, and the small-group plans cover about 21,000, she said.
Access Health’s figures differ somewhat, but still show that Anthem has the largest network of any plans sold on the exchange, with nearly 18,000 providers. By contrast, Access Health figures show the ConnectiCare Benefits network has nearly 11,500 and HealthyCT’s network has just under 7,000.
The figures were reported in mid-February.
According to HealthyCT, the company’s network is now at about 10,000 providers.
How to avoid confusion
Tracy advised that people work with an insurance broker or be sure to be precise when searching online to make sure they’re using the correct network.
Veltri urged people to check whether a particular provider is covered, not just whether a practice is. Her office had a case recently in which an orthopedic group was listed as participating in an insurer’s network, but one provider in the group wasn’t.
“I just think it’s a difficult time. People are having a difficult time navigating right now with the network lists, and we need to help people,” she said. “We ask people who are uninsured to come in and purchase products, and we need to be assuring them that the information they’re getting is accurate.”