The COVID-19 pandemic is subjecting state governments everywhere to an unprecedented stress test.
Victoria Veltri
CT hospitals collect $1.2B in outpatient facility fees over three years
Connecticut hospitals and health networks have received an estimated $1.2 billion in outpatient facility fees from 2015 through 2017, according to data announced on Tuesday. These fees are collected for a wide-range of services, including oncology, eye surgery, psychotherapy and primary care, provided at off-site facilities run by hospitals and health networks.
Small community hospitals struggle to avoid a downward spiral
Many in health care say joining larger systems is key to small hospitals’ survival. But some policymakers are wary of the trend, saying it can raise prices without necessarily improving quality. And leaders of the state’s few remaining independent community hospitals say their organizations are facing stresses that could jeopardize their viability.
The health care that happens outside the doctor’s office
A few years ago, Nadia Lugo went door-to-door in Hartford’s North End with a list of names and a mission: Find people who were going to the emergency room frequently. Figure out what was keeping them from staying healthy or getting the right kind of care. And try to help. It was the kind of work many in health policy now view as key toward improving the outcomes of high-need patients. But incorporating it into the health care system remains a challenge.
With Obamacare’s future uncertain, CT exchange contemplates strategies
One person likened it to looking at a “foggy crystal ball.” Another spoke of changing a tire on a car that’s still moving. But others cautioned against speculating and emphasized the fact that, so far, nothing about the Affordable Care Act has changed.
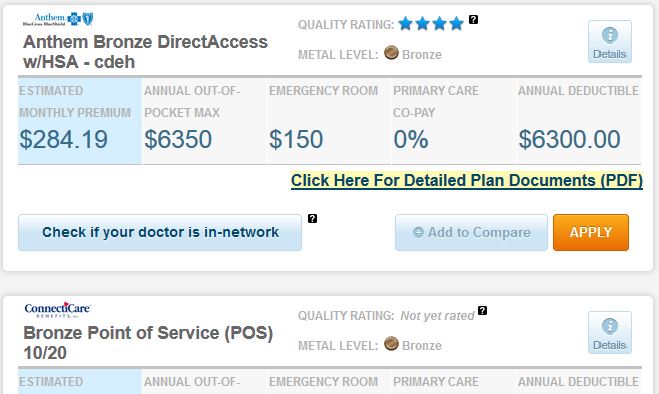
How to manage a high-deductible health plan
High-deductible health plans, which are increasingly common, don’t just require people to pay more when they get care; they also leave people with more to understand, from figuring out how much care costs to handling bills that aren’t always clear. Here are some tips from experts on how to manage a high-deductible plan. This story is the latest in a series on how to better navigate the health care system.
Do public hearings influence what health insurance costs?
A Fairfield County couple traveled to Hartford in June to urge regulators not to let their son’s insurer raise its rates. A month later, the insurance department rejected the company’s proposal. But what role did the public hearing have in that decision? Not much, according to the department.
Obamacare glitch leading to canceled policies, some say
Republican leaders say constituents have had their policies canceled because of problems with the state’s Obamacare exchange. Their claim isn’t entirely accurate, but people involved in insurance administration say problems are causing some people to lose coverage.
Patients will get notices about ‘facility fees’ starting in October
Starting in October, patients will receive advance notification if they will face extra charges for getting outpatient care at hospital-owned facilities, under a bill Gov. Dannel P. Malloy signed into law.
Healthcare advocate wants hearing on Anthem rate request
State Healthcare Advocate Victoria Veltri has asked the Connecticut Insurance Department to hold a public hearing on Anthem Blue Cross and Blue Shield’s proposal to raise premiums for its individual-market health plans by an average of 12.5 percent next year.
The Basics: CT’s effort to notify patients of added medical fees
The state House Wednesday passed a bill aimed at making sure patients know about “facility fees,” extra charges they could face if they get outpatient care at medical offices owned by hospitals.
Latest Obamacare confusion: Exchange plan provider networks
The rollout of the federal health law in Connecticut has been smoother than in many parts of the country, but it hasn’t been without hiccups. The latest one: finding providers who take the new coverage.
For some new Medicaid clients, delays getting care, prescriptions
People who are deemed eligible for Medicaid get a letter to use as proof of coverage until their insurance ID cards arrive, but some have found that pharmacies and doctors won’t accept it, leaving them unable to get care or medication.
Feds consider scaling back Medicaid estate recovery
For some adults, getting Medicaid coverage means that when they die, the state could claim some or all of their assets to repay the medical care they received. That’s left some people who qualify for the program under the federal health law wary of joining. And now the federal government, concerned about the effect on enrollment, plans to explore scaling back the practice.
CT hospitals’ group recommends notifying patients on facility fees, costs
As state officials push for legislation, the Connecticut Hospital Association has recommended that its members provide patients with specific information about “facility fees” they could incur if they get care at hospital-owned medical offices.