Mubarak Soulemane’s mind was racing the day a state trooper shot him seven times. It wasn’t the first time he’d had a manic episode. His family would frequently call the New Haven police to help the 19-year old when he was in emotional distress.
His sister, Mariyann, estimates the cops took the teenager to Yale New Haven Hospital ten times since he first started showing symptoms of mental illness in 2016.
“It was a constant battle: Mubarak versus schizophrenia,” Mariyann said.
Soulemane was in the throes of a mental health crisis this past Jan. 15, when he allegedly threatened people with a knife inside an AT&T store and then stole a car in Norwalk. Chased by police, he sped down I-95 at around 90 miles per hour, according to police footage, until he was pulled over in West Haven. State Police Trooper Brian North exited his car, removed his gun from its holster and pointed it at Soulemane, still seated in the car behind a closed door, reportedly holding a knife. After about 30 seconds, per police videos from the scene, Soulemane appeared to shuffle in his seat. North fired his weapon several times into the driver-side window, killing Soulemane.
“State police should have been notified, ‘This is a missing person with underlying mental health issues,’ so they can then know how to proceed,” Mariyann says now. She believes the state trooper failed to recognize her brother’s emotional distress, that what he needed to show Soulemane that day was compassion and care, not his gun. “He panicked and pierced my brother’s body with bullets.”
Soulemane’s death at the hands of a white police officer is one of the many tragedies feeding a growing anger about the way this nation’s police officers threaten, and ultimately harm, black lives, as well as those of other minorities. The tipping point came last month when George Floyd, a black man police suspected of passing a counterfeit bill, was suffocated to death while handcuffed face down on the pavement as a white Minneapolis officer kneeled on his neck for almost nine minutes.
It’s not reasonable to expect cops to be social workers and the people who direct traffic.”
Floyd’s death, which was captured on video, has led to protests in cities and towns across America and forced a reckoning about the role of police in American society. On the streets and in Zoom calls, protestors and lawmakers are grappling with the racism and militarization inherent in many of the nation’s police forces, and what happens when those factors overlap with the growing array of roles police officers play in society.
One of the more problematic roles is that of first responder for mental health crises — a job for which most officers are ill-equipped and which, as Soulemane’s death illustrates, can lead to disastrous consequences. Police officers in Connecticut have killed 21 people in the past five years, at least five of whom suffered from mental illness.
The question being asked by reformers and police across Connecticut is how to move forward. Should officers receive more mental health training or should funds instead be allocated to community supports so those in crisis don’t have to rely on an armed police officer to deescalate the situation and direct them to a mental health professional?
“It’s not reasonable to expect cops to be social workers and the people who direct traffic,” said Dr. Eden Almasude a psychiatrist at Yale New Haven Hospital. “Police involvement in mental health care makes people worse, not better.”
It wasn’t always this way. Cuts to the social safety net and the deinstitutionalization of patients from psychiatric hospitals from the 1960s through the 1990s have forced police to be more than guardians of public safety. They are often the first to respond to people dealing with complex issues, like homelessness, mental illness and unaddressed trauma.
“Throughout the years as our structures have reduced funding for social programs, educational programs, mental health programs, the void is filled by law enforcement,” said Keith L. Mello, chief of Milford Police and head of the Connecticut Police Chiefs Association.
But change is possible. Amber Kelly, a clinical social worker based in New Haven and an assistant professor at Quinnipiac University, said it is a “failure of imagination” to rely on police to solve such nuanced social and public health dilemmas.
“We need to come up with systems other than policing to deal with these social problems.”
An unkept promise and a new role
To save money and decrease reliance on large psychiatric institutions, the administration of Gov. John G. Rowland closed Fairfield Hills and Norwich State hospitals, in 1995 and 1996. Rowland and other state officials pledged to fund community-based mental health services when the facilities closed, but that never happened. To this day, advocates are still waiting for local, state and federal governments to provide the comprehensive supports that were promised.
“Many of the people that we knew are now in prison,” said Karen Kangas, the director of Recovery and Family Affairs at Hartford HealthCare. “Many people who really were in need had to be taken by police to jails and prisons for misdemeanors, because there were no longer places in hospitals for them to go.”
The hospital closures and lack of community-based care have forced police to work on the frontlines of the mental health crisis. But cops are not social workers, Thomas Kulhawik, chief of the Norwalk Police Department, told the Police Transparency and Accountability Task Force earlier this week. “They’re not trained to be. Police officers act in that capacity. But that’s one aspect of their job.”
Most law enforcement officers get very little training on how to respond to people in mental health crisis compared to the instruction they get on using a firearm or defensive driving, said Lorenzo Boyd, a former sheriff’s deputy and current associate professor and director of the Center of Advanced Policing at the University of New Haven.

“The police know how to do two things really well: detain and use force,” Boyd said. “So that’s the prism through which they view all the problems they deal with: can we arrest, or can we detain?”
Roughly 50 of the 900-plus hours municipal police officers spend in basic training deals specifically with mental health, said Karen Boisvert, police academy administrator with the Police Officer Standards and Training Council.
“It’s difficult to put an exact hour on it because while there are courses [explicitly] dedicated to mental health treatment, it permeates throughout the program,” said Mello, explaining that once the recruits finish the classroom work, they get another 400 hours of training in the field. “You shouldn’t assume that’s the only mental health training they get.”
I don’t think we have any option but to be social workers, marriage counselors, coaches. Unless you can make people perfect and have no mental health issues, I think it’s inevitable police officers are going to be on the front line …”
Still, Mello acknowledged, “You’re not training specialists in anything.”
In addition, police departments can have their own crisis intervention training programs, if they are locally or regionally funded. The Waterbury Police Department, for instance, started their own initiative around the mid-2000s. Chief Fernando C. Spagnolo said officers work with licensed clinicians who respond to crises between the hours of 6 a.m. and midnight. Officers develop relationships with community members they help who are in mental distress, a vital skill considering the frequency with which Waterbury police work intersects with mental health issues.
“It’s a big part of our job, and it’s not going to go away,” said Spagnolo.
Veteran officers can also meet their certification renewal requirements by taking more mental health training courses, provided by private companies like Blue Courage, Mental Health First Aid or the Connecticut Alliance to Benefit Law Enforcement.
Officers’ training doesn’t just stop once they leave the academy, said Joann Peterson, a retired New Haven Police captain who is now a training officer at the Connecticut Police Academy. In fact, it’s vital that they continue to learn that “an arrest is not always the right solution,” considering how often cops interact with someone with a mental health condition.
“I don’t think we have any option but to be social workers, marriage counselors, coaches,” Peterson said. “Unless you can make people perfect and have no mental health issues, I think it’s inevitable police officers are going to be on the front line, to recognize [a mental health crisis] and then get people to the right place.”

A need for training?
Even with all the training available for police officers in Connecticut, there are limitations in their ability to respond to situations where people are in a mental health crisis. By Mariyann’s account, the New Haven police were helpful when they interacted with her brother, but “it didn’t really require much. Their best efforts were to lure him in the ambulance and take him to the hospital.”
Connecticut is a small state, only 4,845 square miles. Someone in emotional distress like Soulemane doesn’t have to travel a great distance to be in the jurisdiction of another police department, one where the cops aren’t aware of their mental health condition.
“You can’t share with all the police departments everybody who’s schizophrenic because that would be a violation of our health laws,” Peterson said.
Daniel Reyes had auditory hallucinations, anxiety, psychosis and paranoia before Thomaston police killed him in June 2016. In an investigation into his death, New Britain State’s Attorney Brian Preleski acknowledged police are required to receive training on how to handle encounters with people who are emotionally disturbed, but suggested the Division of Criminal Justice could partner with law enforcement to determine whether the training is consistent with best practices.
“This is not, nor should it be interpreted as a criticism of the Thomaston Police Department or any of its members. It is an issue common to virtually every small police department in Connecticut,” Preleski wrote. “One result of Connecticut’s preference for local government is a proliferation of small police departments that lack the resources to ensure that trained [Crisis Intervention Team] patrol specialists are available to respond as needed.”
Police officers across Connecticut also use non-lethal force on those experiencing a mental health crisis. According to a 2017 analysis conducted by Central Connecticut State University’s Institute for Municipal & Regional Policy, more than one-third of people tasered by law enforcement were “emotionally disturbed.” Those described that way were more likely to be tasered than those who were not emotionally disturbed.
Almost half of those tasered by police were under the influence of drugs or alcohol, or were thought to be intoxicated.
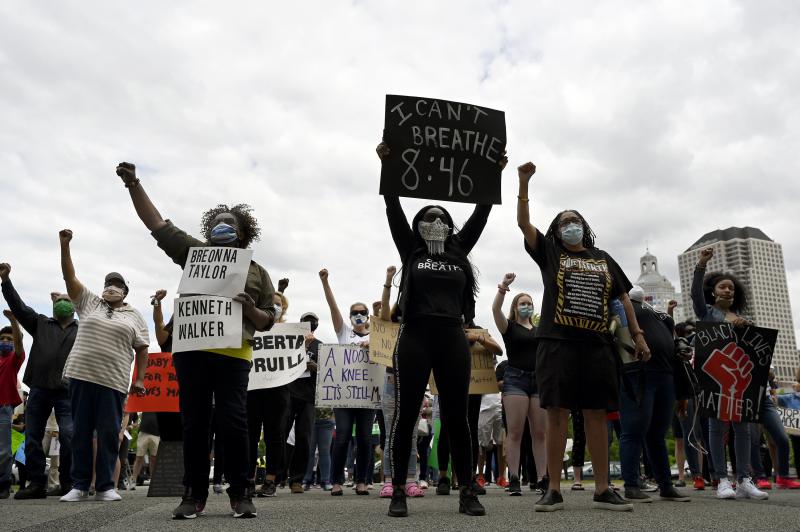
Mariyann started a petition that has garnered more than 75,000 signatures demanding police receive in-depth training on racial bias and how to interact with people who have a mental illness. It also calls for funding for community organizations. Kira Ortoleva, head organizer for the group Justice for Mubarak, said there should be special units of mental health professionals that assist police on an as-needed basis.
“Medical professionals would be able to tell whether excessive force is being used against a patient, or somebody who is being arrested,” said Ortoleva.
Similar intervention services already exist through state and private entities, though they’re not always available or come with restrictions, such as only serving children. In addition to 14 mobile crisis response teams scattered across Connecticut, The Department of Mental Health and Addiction Services has five crisis intervention clinicians through state-operated local mental health authorities. They could ride with police to help people in a psychiatric emergency and deescalate situations where people are in crisis so they can be referred to needed services.

Many question whether any amount of training will make police qualified to help someone in a mental health crisis. After all, in Minneapolis, the city where Floyd was killed, police officer receive 40 hours in Crisis Intervention Training. Others are suspicious of joint responses to someone in emotional distress, where cops and mental health professionals work in tandem.
“The aim of our responses should be addressing harm, uplifting healing and true safety that does not rest on state violence,” Jeannia Fu, a community organizer with CT Bail Fund who studied at the Yale School of Public Health. “More generally, I believe, as someone in public health, that health care workers need to sever their relationships to police and the carceral state.”
… Or an investment in community mental health services?
Many of Almasude’s patients at Yale New Haven Hospital’s psychiatric emergency department are brought in by police. Some are handcuffed to the bed, bound the entire time they’re there. Almost every one of them has experienced violence and trauma in their lives, she said; it is retraumatizing to be in close quarters with armed individuals who have a history of killing those with mental illnesses. A police officers’ “mere presence” at the scene of a crisis is enough to escalate the situation, said Almasude.
“Imagine what it might be like to have a psychotic episode and be met with guns, to be handcuffed, treated inhumanely, put in the back of a police car, and then dumped at the hospital,” Almasude said. “Everything about that process is inhumane and because there’s so much discrimination against people struggling with mental health, that is seen by a lot of people as acceptable.”
Police are particularly ill-equipped to deescalate situations where people are in a mental health crisis, said Kelly, the New Haven-based social worker. Those in emotional distress should be given a series of choices, Kelly explained, providing them agency and control. That flies in the face of law enforcements’ default disposition for managing a crisis.
“The way they are trained is to establish control in the situation, and almost every time that’s going to escalate a mental health crisis,” said Kelly.
When people say ‘abolish the police,’ they don’t mean that no one will respond to a call for help in a crisis. It means we need to redirect the funding that goes to the police departments toward community-based solutions.”
“It’s more likely the person in crisis will be harmed than that they will do harm,” Almasude said. “There’s no amount of training that can lead a police officer to respond appropriately to someone in a mental health crisis.”
One potential solution are mobile crisis units that don’t work with the police, available all across Connecticut 24 hours a day, seven days a week. The response team would be made up of mental health counselors trained in de-escalation techniques. That way, police don’t enter into the situation at all when someone calls 911 because of psychiatric distress.
“A person who is a trained mental health worker is far more able to de-escalate that situation and have everyone come out of the situation safely and directed to appropriate care,” said Almasude.
“When people say ‘abolish the police,’ they don’t mean that no one will respond to a call for help in a crisis,” she added. “It means we need to redirect the funding that goes to the police departments toward community-based solutions.”




I believe strongly in the need for reform. Defunding Police Departments will only create more problems as racism is manifested in so many other ways. I have a daughter that has mental issues along with a substance abuse problem. She was approached by the Nhpd on several occasions for the same violation; driving without a license, etc. Nor did she ever have an ID. The officers were so used to seeing her they stopped writing her up. When her condition got to a point we couldn’t take her anymore I had to write an email to the department and ask them why no legal action had been taken. We needed their help to implement the fear of the law and consequences too. They stopped her again and she finally was arrested and incarcerated. This saved her life. So de-escalation should be part of training.
Hi Diana, thanks for your submission. We’re happy to publish it. That said, please make sure to sign future comments with both your name and town, as required under our new comments policy.
Great article but what is missing is the recommendation that police departments employ social workers directly or contractually. Larger departments can achieve the former and smaller departments the latter. Social workers can provide training, go out on calls where mental health and social factors are involved, use de-escalation techniques, and as part of the department help to develop policy reform. There is an ample social work workforce to find qualified candidates and money that is taken from defunding initiatives can be instead reallocated for employment of social workers.
Stephen Wanczyk-Karp, Cromwell
Kurt Kaufman, Putnam, CT
My concern, having seen patients experiencing psychotic episodes in the hospital ER, is that people may be hurt (unintentionally, though it may be) by such patients during attempts to redirect them and calm them. My fear is that, after a few persons are seriously injured in their attempts to do so, it will be recognized that you need both skills, i.e. mental health and defensive. This may be a difficult combination of skills to find in mental health professionals.
I’ve taken the Mental Health First Aid course mentioned in the article and recommend it to everyone, not just first responders. Even if you never put it into practice, the understanding you will gain about people with mental health issues is worthwhile.
Hi Mark, thanks for your submission. We’re happy to publish it. That said, please make sure to sign future comments with both your name and town, as required under our new comments policy.