Six months have passed since Maria has stepped outside Yale New Haven Hospital.
No fresh air. No wind, rain or sun on her skin. No home-cooked meals. Just air conditioning, lukewarm cafeteria meals and the view from her window, overlooking the hospital’s parking garage.
There’s also access to the dialysis treatment she needs. Without it, her doctor gives her only a few days to live.
If she goes home, she won’t be able to go for dialysis at a clinic or another less-expensive program, because she is an undocumented immigrant.
So Maria is stuck in the hospital, despite being well enough to leave YNHH and get outpatient dialysis. Her only other alternative is to leave and return to the emergency room every few days when her kidneys start shutting down.

“I just want to leave here right now. I’m bored,” said Maria, who checked into the hospital Dec. 8 when her kidneys began shutting down. “Before, I thought my life was ending, and that’s how I feel now that I am trapped here … I consider being here even worse than being in jail. They tell you you can’t go out. Just look out the window.”
The CT Mirror is not disclosing Maria’s real name at her request because she is undocumented.
Hospitals are required by federal regulations to provide life-sustaining treatment to uninsured undocumented immigrants who show up in the emergency department and to treat them until they can be discharged safely. In Connecticut, however, undocumented immigrants don’t have access to outpatient services or less-expensive nursing home care if they require ongoing treatment after hospitalization.
So patients like Maria must stay in the hospital to stay alive.
This is both extraordinarily expensive and, in the view of civil rights attorneys, a form of “humanitarian incarceration.”
“Allowing someone to die an agonizing death — or go through repeated rounds of severe, terrifying acute symptoms, followed by an ER visit, in-patient admittance and then stabilization and discharge, to be repeated again just days later — cannot be what Connecticut citizens expect of their government,” a coalition of legal aid attorneys wrote top officials in Gov. Ned Lamont’s administration on April 27.
The Department of Social Services declined to comment on the state’s policy not to cover certain life-sustaining outpatient services for undocumented immigrants and legal immigrants who moved here within the last five years. Medical care for these patients stuck in the hospital is paid for with a combination of state and federal dollars through Medicaid. Since dialysis hasn’t made Connecticut’s list of covered medical care, undocumented immigrants are unable to access treatment unless they show up in the emergency room.

The legal aid attorneys from New Haven Legal Assistance Association, Greater Hartford Legal Aid and Connecticut Legal Services also have not heard back from the Lamont administration.
Failure to cover the treatment comes at a steep cost to taxpayers.
The cost of Maria’s six-month hospital stay is now more than $1 million, her legal aid attorneys estimate, compared to roughly $91,000 a year for outpatient dialysis treatment.
The state and federal governments are picking up the bulk of that bill, since undocumented immigrants qualify for Medicaid when they require life-sustaining measures in the hospital. At least 14 other states cover outpatient dialysis treatment, including Massachusetts and New York.
An unquantified problem
National estimates suggest that somewhere between 5,000 and 9,000 undocumented people in the United States have end-stage kidney failure, which necessitates dialysis.
Connecticut officials do not know how many of these “permanent patients,” as some hospital officials call them, are being subsidized by the state to live in the hospital. Nor do they know how much Connecticut could save by allowing Medicaid to cover outpatient dialysis and other step-down treatments for certain chronic health conditions.
Civil rights attorneys and Senate President Pro Tem Martin Looney, D-New Haven, believe there are other undocumented immigrants trapped in Connecticut hospitals on any given day.
“I do not believe that [Maria] is the only patient in Connecticut in this situation,” Looney wrote the state’s commissioner of the Department of Social Services on May 25. “This policy seems not only inhumane but also financially unsound. Allowing Medicaid coverage for outpatient dialysis would allow this patient to go home, and it would also save money for the state. I urge you to make this change as soon as possible.”

Yale New Haven Hospital declined interview requests and did not respond to specific questions for this story.
Hartford Hospital officials said they have decided to cover the cost of outpatient dialysis so that those who need the treatment can be discharged without delay. The hospital currently is paying for 10 undocumented patients to receive outpatient dialysis, which costs about $520 per treatment. The annual cost for the hospital to cover this is $270,000 a year.
“We don’t have to keep our patients in the hospital for a long period of time waiting to find a place that will take them, or figuring out a way to fund that,” said Dr. Suparna Dutta, chief of medicine at the hospital.
The hospital does struggle, however, to discharge some undocumented immigrants who don’t necessarily need to remain in the hospital but aren’t stable enough to return home and could benefit from a nursing home or less-expensive setting to receive care.
“They’re fine in terms of their medical issue. They don’t need to be in the hospital anymore, but then the issue kind of becomes, where do they go next?” Dutta said. “Sometimes our recommendation is a care facility so they can get stronger before they go home, so you don’t worry about them going home and falling. But, obviously, if you don’t have insurance, that gets quite expensive. So where you don’t have the option of sending your patients to a more controlled setting, then sometimes you’ll keep them in the hospital a bit longer until you’re absolutely sure that they’re going to be OK at home.”
It is unclear just how widespread this problem is, although Dutta suspects that undocumented immigrants disproportionately require dialysis treatment. That’s because undocumented immigrants often don’t have private insurance, don’t qualify for Medicaid, and therefore are unable to get a kidney transplant to avoid a lifetime of dialysis treatment. Dutta suspects that they also struggle to access the medications necessary to avoid eventually requiring dialysis.

Community health centers, which serve as a safety net for vulnerable populations, struggle to fill the void.
Dr. Ben Oldfield, the chief medical officer of Fair Haven Community Health Center in New Haven, said people with diabetes too often land in the emergency department because of a lack of access to insulin and an endocrinologist. One out of every four patients who come to his clinic are undocumented immigrants.
“We have certain resources to get our patients specialty care through certain programs, but oftentimes those programs depend on this condition that [the patient’s] condition be life threatening,” he said. “If they are uninsured [and need to see an endocrinologist], we don’t have a lot of recourse to make that happen … They don’t get the care they need, and then there is a greater likelihood of ending up in the hospital.”
The constraints placed on treatment by the medical system have adverse effects on the quality of care that undocumented patients receive; a study of undocumented immigrants with end-stage kidney failure found that those who receive dialysis only in emergencies had a mortality rate that was 14 times higher. Undocumented immigrants also face financial barriers in receiving kidney transplants, which are considered the best course of treatment for the condition.
Annual efforts to expand access to the state’s Medicaid plan — known as Husky — have failed to win approval by the General Assembly. However, the Democratic-controlled legislature has sent a bill to the governor’s desk to open the door for the children under age 8 this year.
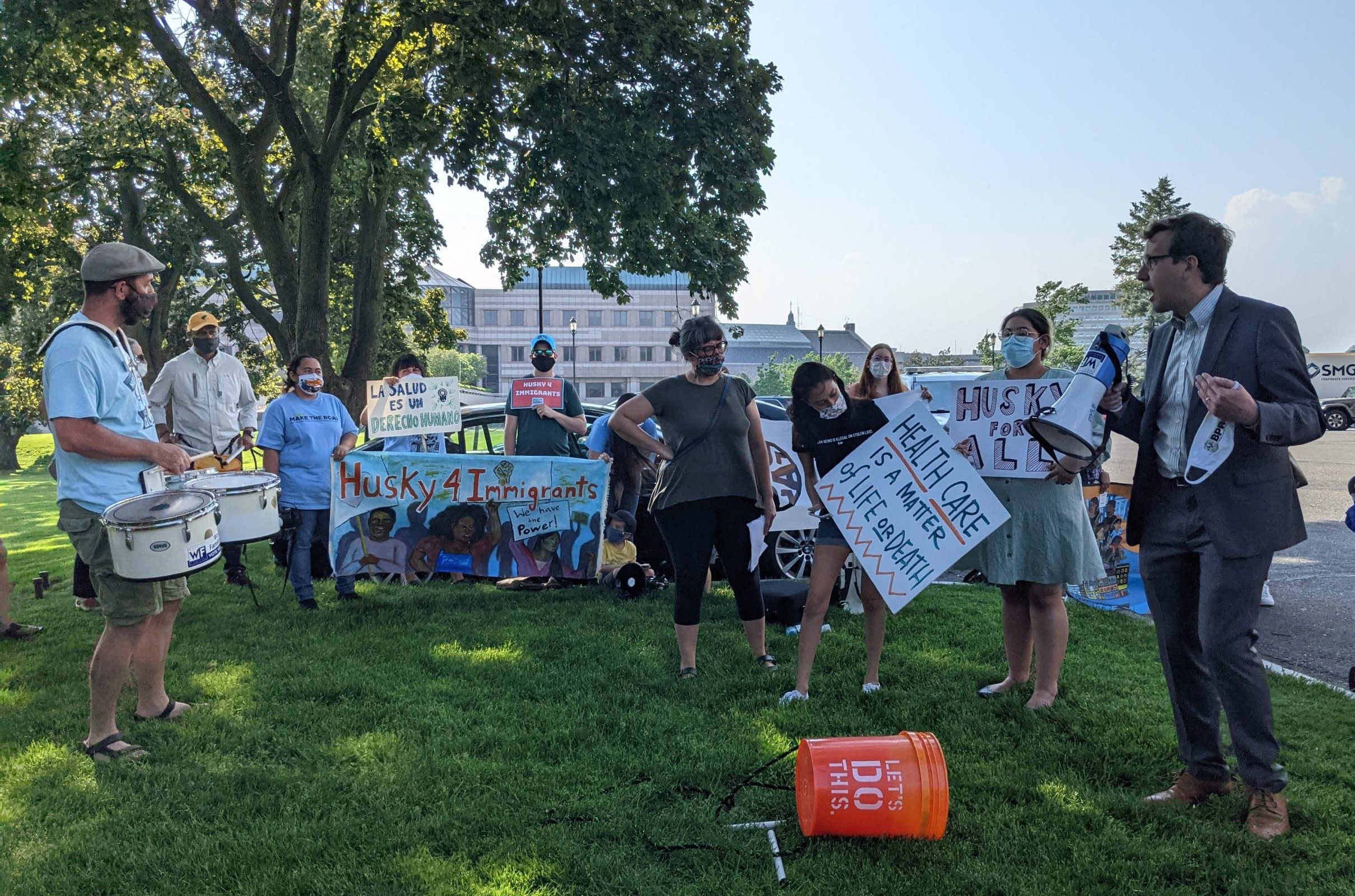
“If there was basic coverage that allows people to get in to see doctors, get preventive care, to have Medicaid coverage if they have newly diagnosed diabetes or high blood pressure, they can start on treatment right away and be monitored closely, and we’re going to have less people that are going to even be admitted to the hospital or needing dialysis or needing to hang out in the hospital waiting for that rehab,” said Dutta.
The Connecticut Hospital Association in a statement said too often undocumented people show up in crisis in their emergency departments.
“No one should have to wait until a medical problem becomes an emergency to seek care. Unfortunately, Connecticut’s hospitals often see cases where delays in care due to lack of insurance or immigration status result in much more serious illnesses, requiring more intensive care and resulting in less positive outcomes. The Connecticut Hospital Association supports extending insurance coverage to low-income, undocumented immigrants living in our state. Investing in earlier, more appropriate access to care means healthier communities and lower cost of care for all.”





