While completing her medical residency in Manhattan, Dr. Manisha Juthani kept circling back to a topic that stoked her passion for science and tapped into her inquisitive nature: infectious diseases.
She still recalls the case of a young woman who came to New York-Presbyterian Hospital with what ultimately was diagnosed as typhoid fever and learning about the intricate process of tracing that transmission to a nearby fast food restaurant.
“I figured out, through what I had heard from the public health department, that there were three different cases in the city. And they were all traced back to one fast food restaurant in Queens,” Juthani said. “They traced it back to one specific worker in that establishment. There are people who can be chronically colonized with salmonella typhi, and they just shed it all the time. And if it contaminates food, it can infect somebody else. It infected three other people that way.”
The detective work it takes to diagnose and treat patients fascinated Juthani, and she found her niche in infectious diseases.
“Whether it’s HIV patients, whether it’s flesh-eating bacteria … I think what it really came down to is the investigation. It’s like being a detective,” she said. “As an infectious disease doctor, you’re sort of the Matlock or Sherlock Holmes of medicine. People’s stories are actually what help determine the diagnosis of the patient. And so listening to stories was something I always appreciated.”
Juthani hopes her keen listening skills and discerning nature will be strengths as she dives into her new role as commissioner of the state’s Department of Public Health, a 682-employee agency that has been consumed by COVID-19 for more than a year.
The state’s last health commissioner, Renee Coleman-Mitchell, was fired just two months into the pandemic, and the head of Connecticut’s social services department took over the role on an interim basis for 16 months until Juthani’s arrival in September. Even prior to that, other state officials, including epidemiologist Matthew Cartter and Chief Operating Officer Josh Geballe, had become the agency’s visage in the early months of the coronavirus crisis.
Coleman-Mitchell has accused state leaders of discrimination, saying she was shut out of important policy decisions, supplanted by others with no public health experience and ultimately dismissed from her job without cause. Gov. Ned Lamont did not give a reason for her firing.
Since she was nominated to her post, Juthani has been visible and vocal on key issues, including her support of a vaccine requirement for nursing home workers who treat some of the state’s most vulnerable people, and her strategy for distributing the COVID-19 shot to young children.
Juthani wades into her position at a time when state and local health departments nationwide have become a target of public ire over vaccine and mask mandates and other restrictions. The agencies are grappling with burnout, terminations and a legacy of underfunding that began years before COVID-19 swept the world but that left many departments ill-prepared for the pandemic. Connecticut’s own agency was criticized for its handling of the crisis in nursing homes, where a majority of the state’s coronavirus deaths occurred in 2020.
Still, health advocates say fresh energy and enthusiasm are needed in public health now more than ever.
“I know it has been difficult for everyone. The work load has been absolutely tremendous over the last two years, not only dealing with all the aggression and politicization of public health issues but also dealing with a workforce that was experiencing the pandemic,” said Raul Pino, who served as the state’s health commissioner from 2016 to 2019. “But this is not the time to quit. The crisis is just wasted if we don’t learn from it, and what we have to do is learn to advocate for public health.”
Despite the turmoil, Juthani is approaching the job with a mix of optimism and mettle. Some of her top priorities are addressing health equity and the effects of climate change on Connecticut’s people, along with boosting participation in the COVID-19 vaccination program. Connecticut has one of the highest immunization rates in the country, but Juthani will still need to coordinate a new wave of vaccinations for young children and oversee the continued rollout of booster shots.
Watching scores of angry protestors trail Lamont and other state officials in public recently gave Juthani pause about taking over the role of commissioner.
“I did think about it,” she said. “But ultimately, I decided that being in service for others and in service at a time where maybe my expertise would benefit the people of our state – this was a time that I could step up to the challenge.”
Winning trust
For the last five weeks, Juthani has walked the halls of the health department’s brown brick building on Capitol Avenue in Hartford, weaving through cubicles and pausing to introduce herself to the staff. When she meets someone new, she’ll sometimes ask them to play tour guide so she can explore new corners of the office.
One-on-one conversations are important. Juthani is trying to win back trust and boost morale among employees who have been without a permanent leader for more than a year, who have put in long hours for months on end and whose confidence in management had wavered even before the pandemic.
A survey of workers early last year highlighted widespread discontent and plunging morale, with some critical of Coleman-Mitchell’s leadership. A volley of retirements and resignations preceded the first cases of COVID-19.
Juthani is trying to restore some of that trust and rebuild her department, though she warned those efforts won’t happen overnight.
“My goal is to create a positive environment, where people feel valued for their contributions on a day-to-day basis,” she said. “I want to create a leadership team and an organization where it’s clear who to go to for what, but that’s going to take a little time. I have heard from multiple people that we need to have more staff. And I agree.”
Part of that will involve building out a talent pipeline with public health colleges across the state, expanding upon programs already in place and devising new ones. Diversifying the workforce is an issue Juthani wants to tackle.
Ultimately, I decided that being in service for others and in service at a time where maybe my expertise would benefit the people of our state – this was a time that I could step up to the challenge. ”
“I can see recruitment with partnerships … and being able to create feeder programs from our public health schools, particularly among members of our Black and brown communities who go to those schools,” she said. “I want our workforce to reflect our community, to reflect the people we are going to be helping and to make a dent in some of those disparities.”
While at the helm of the department, Coleman-Mitchell was criticized for her reluctance to offer a professional opinion on certain public health topics, including a controversial proposal to remove the state’s religious exemption from mandatory school vaccinations, a measure that ultimately won passage in the legislature this year.
Coleman-Mitchell was the first health commissioner to publish school-by-school data on vaccination rates. But after igniting controversy with the release, she refused to disclose subsequent school-level data. Her decision was overruled by the governor.
“Prior commissioners have embraced their role as experts in offering information and guidance to the General Assembly, which is one of the things we expect of the public health commissioner,” Senate President Pro Tem Martin Looney told The CT Mirror in a 2019 interview. “I certainly think the unwillingness to offer her professional expertise on these issues is of concern.”
Juthani said she is comfortable offering her opinion. During a press conference in July announcing her appointment, she expressed support for a requirement that nursing home workers be vaccinated against COVID-19. In an October interview with the CT Mirror, she said she would favor a coronavirus vaccine mandate for school-aged children once the shot receives full approval from the U.S. Food and Drug Administration.

Her opinions made headlines even before she was named health commissioner.
Last December, Juthani and several other physicians wrote a letter to Lamont urging him to close restaurants and gyms as COVID-19 cases crept back up. Juthani relayed that she was familiar with three cases of the virus that had spread by people who had dined together.
“What I know is that certainly meal times are a major, high-risk event where transmission of this virus can occur,” she said during a COVID-19 briefing with Lamont.
Firm but sensitive
Juthani, 48, is the daughter of two doctors who moved to the United States from Mumbai, India in 1970. She was raised in Greenville, N.Y., commonly known as Edgemont.
She earned an undergraduate degree from the University of Pennsylvania, attended Cornell University Medical College and finished her residency training at New York-Presbyterian Hospital Weill Cornell Campus.
Juthani started at the Yale School of Medicine in 2002 in an infectious disease fellowship and joined the faculty full-time in 2006. Six years later, she was named director of the infectious disease fellowship program.
At Yale, she focused on managing and preventing infections in older adults. She also studied the intersection of palliative care and infectious diseases.
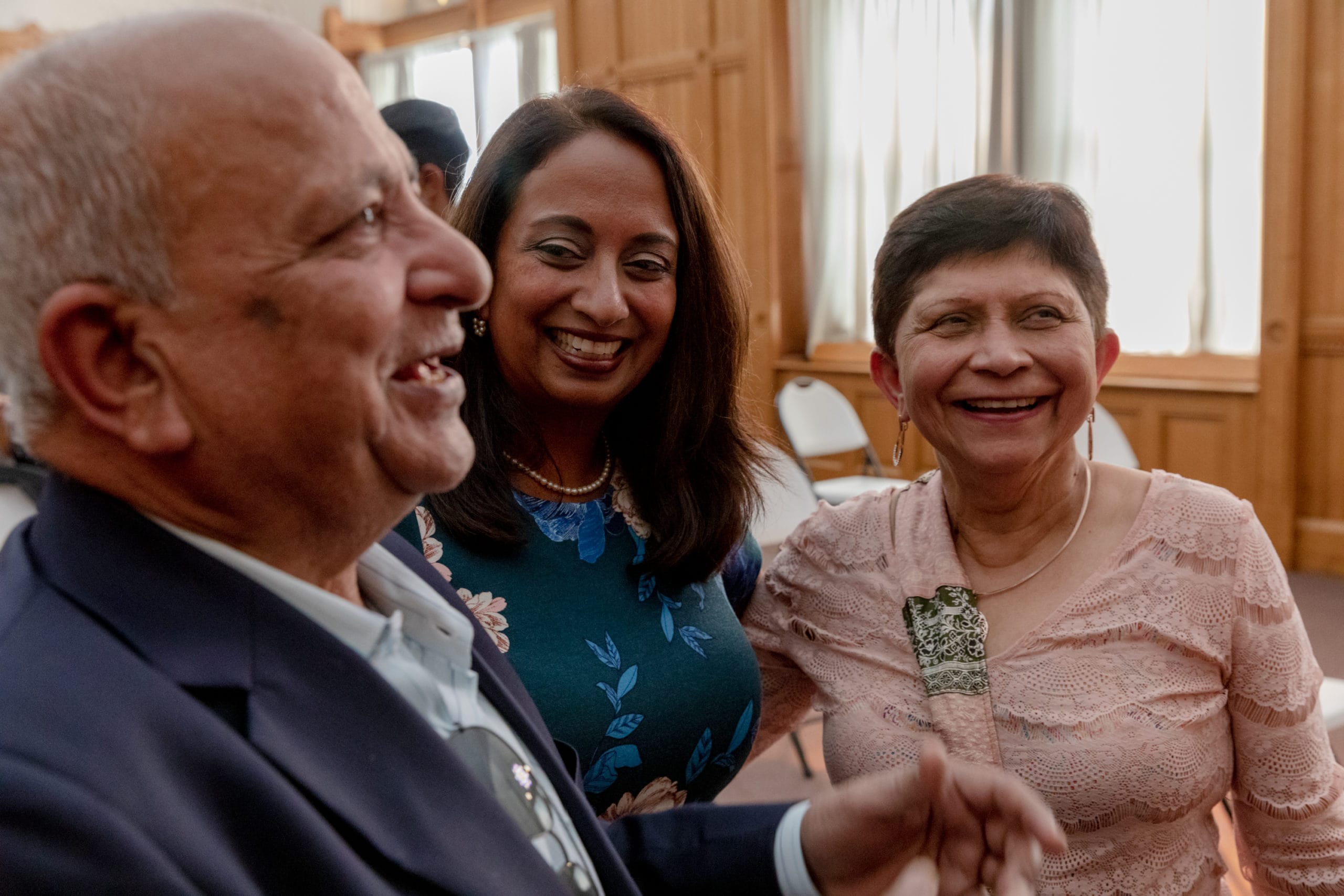
When she was named commissioner on July 26 – the first Indian American person to take up such as a position in Connecticut state government – her parents, Dr. Virendra Juthani and Dr. Nalini Juthani, attended the ceremony, as did many other family members and friends.
“I have lived a very blessed life, I would say. My parents came here with $8, but they had education in the bank. And in America, education gets you a long way,” Juthani said. “I started out with very little, but my parents worked hard and were able to provide for me and my siblings, and [for] my education. That was something that was always prioritized as a family. I grew up with that value.”
The mother of two, who lives with her husband in Fairfield, was chosen from more than 100 candidates nationally. She will be paid $210,000 annually.
Dr. Albert Ko, an infectious-disease physician at the Yale schools of Public Health and Medicine, described Juthani as a kind, attentive doctor. As director of the fellowship program, she served as a mentor and guide for new physicians.
“Actually coming from the patients, they tell me what a wonderful physician she is in terms of being caring, but also sensitive,” said Ko, who served as an adviser to Lamont during the pandemic. “I also know about Manisha from the infectious disease fellows, the ones who we are training. Manisha really knows the right thing to say – how to give the right advice at the right time. She’s firm, but sensitive. She has that very special skill.”
Along with managing the ongoing pandemic, Juthani wants to use her current role to focus on health equity, including disparities in access to health care, and the effects of climate change.
Part of that approach is bringing an “equity lens” to all efforts underway at the health department, she said.
“Every single one of these topics that we do needs to be looked at with an equity lens. If you go in with that mindset, you can start to generate data and you can potentially identify where those areas of additional work need to be done,” she said.
Juthani has already begun to take a deeper look at how COVID-19 has affected the state’s communities of color, especially in case rates and vaccination initiatives.

“We’re looking at what gaps still exist. I know offhand that a lot of the younger groups are still the groups we need to target, particularly among our African American communities, and use that to inform how we move forward,” she said. “We’ve actually done so well as a state. … If you look across the age spectrum, there are many older people in Black and brown communities who’ve gotten vaccinated. But I think we have work to do still in younger communities.”
As the pandemic put a spotlight on health disparities that existed long before coronavirus arrived, the legislature responded this year by passing a sweeping bill declaring racism a public health crisis, mandating better data collection on race and ethnicity in health care and requiring hospitals to conduct implicit bias training for employees who provide direct care to pregnant and postpartum women. The bill includes several other provisions, such as establishing a commission on racial equality in public health.
But when health disparities are no longer in the spotlight, advocates say public health leaders like Juthani must continue to tackle them.
“Prevention and clinical work and addressing what we call social determinants of health have critical outcomes,” said Pino, who is now the health officer for Orange County in Florida. “These disparities that we saw in vaccination rates and in infections and death rates – who was getting sick and who was getting treated – were also an expression of the health disparities that we’ve had for years existing in our communities. We need to respond to that.”
The health department recently received a $1.5 million, five-year grant from the Centers for Disease Control and Prevention to explore the effects of climate change in Connecticut and create strategies to deal with them.
Juthani has plans to establish a new unit within her department dedicated to the health impacts of climate change. Part of the effort will involve a partnership with the Yale Center on Climate Change and Health. Juthani will hire additional people to work on the state side of the project.
“Climate is going to dictate our future,” she said. “We see it every day in our lives, in the way it has impacted things.
“Losing heat or air conditioning, food insecurity – all of these things are often related to extreme weather. And it comes back to equity.”

Through the worst?
While substantial problems lie ahead, Juthani said she believes the most challenging parts of the pandemic are behind us.
“I do think we’re through the worst,” she said. “We have a very vaccinated state, but we still have work to do. People who are eligible for boosters should get them. It will help prevent breakthrough cases. But I think we’re in a much better place than we were.”
The focus now will shift to a wider distribution of booster shots and the rollout of the COVID-19 vaccine for 5- to 11-year-old children. In Connecticut, 277,630 children recently became eligible for the immunization, and the first shots were administered less than an hour after federal authorization.
Juthani tapped a network of pediatricians and pharmacies to prepare, and the state so far has ordered 96,900 doses of the children’s vaccine.
For now, she does not think Connecticut will go back to the tight restrictions it imposed at the height of the pandemic, when masks were mandatory indoors and swaths of the economy were shuttered.
But residents should remain vigilant to avoid another cold weather swell in cases, she said.
“We’ve seen in some of our more northern states, which are colder than us, that their rates did go up. That makes me worried that as it gets colder here, we could have more circulation of virus,” she said. “But I do think hospitalizations should be manageable, which at the end of the day is what dictates how things go.
“I just hope we can pull a few more people into the vaccination pool.”



