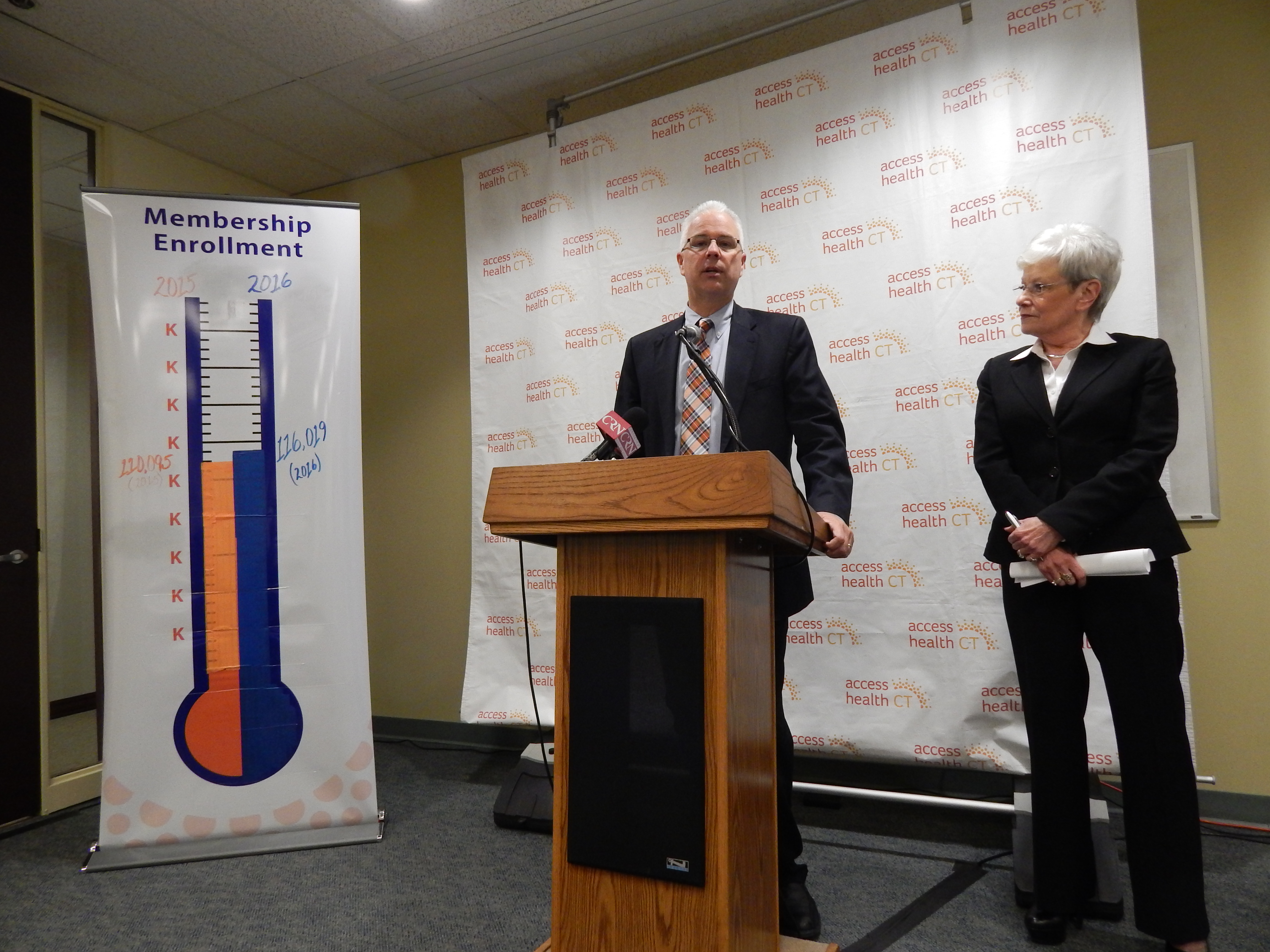Exchange customers who signed up for 2017 coverage and get federal help discounting their premiums will save a couple of dollars each month compared to what they pay now. But for those who don’t qualify for financial aid, costs are rising an average of $76, and for some, that’s after switching to plans with less coverage.
connecticare
As ACA faces new challenges, fixes not assured
WASHINGTON — The Affordable Care Act is facing more challenges than at any time since its initial enrollment period in 2013, when the program was bedeviled by technical glitches. Besides rising premiums and fewer choices in Connecticut and elsewhere, there’s uncertainty a new Congress and a new administration will make fixes to the ACA that will improve its health.
What you need to know for the 2017 Obamacare open enrollment
If you buy health insurance on your own, or plan to, your chance to sign up for 2017 coverage starts next week. Here’s what you need to know, whether you’re new to the process or buying again.
ConnectiCare opens first health insurance store in Manchester
The store, in a 6,000-square-foot former brew pub space, is the first run by a health insurance company in Connecticut, but there’s precedent in other states.
ConnectiCare will stay on CT health exchange in 2017
ConnectiCare, the single-largest insurer on the state’s health exchange, announced Tuesday it would participate in the exchange in 2017 working with the rate schedule the Insurance Department approved earlier this month. That decision means two of the four companies that have sold policies through Access Health CT will participate again next year.
ConnectiCare’s role in 2017 health exchange stuck in legal limbo
The question of whether the largest insurer on Connecticut’s health insurance exchange would participate in 2017 fell into legal limbo late Monday afternoon. Whether ConnectiCare participates next year could hinge on how the state Department of Insurance resolves a new administrative appeal of its recent insurance rate awards.
ConnectiCare could become third insurer to exit exchange today
It has been a tumultuous year for Connecticut’s state health insurance exchange, but the latest – and most significant – blow could come Monday if its largest insurer decides not to offer plans next year.
CT health insurance rates to rise sharply in 2017
Most Connecticut health insurance plans will undergo steep rate hikes next year, although in some cases, the prices will not go up by as much as carriers had sought.
Health insurers face outcry over requests for sharply higher rates
After proposing sharp rate increases for next year’s health insurance plans for individuals and small groups, a trio of insurers faced a barrage of criticism from elected officials and the public during a series of hearings Wednesday and Thursday.
Major health insurers seek sharply higher rates in Connecticut
Some of Connecticut’s major health insurers are seeking rate increases far beyond medical inflation, including an average increase of 26.8 percent for the individual plans offered by the state’s biggest insurer, Anthem Health Plans, according to requests released Monday. The filings come as the insurance industry, state Insurance Commissioner Katharine Wade and her department are under intense scrutiny over proposed mergers.
116,019 CT residents signed up for Obamacare plans
Updated at 6:50 p.m.
In all, 116,019 Connecticut residents signed up for private insurance through the state’s health insurance exchange, Access Health CT, during the open enrollment period that ended last week, officials said Monday.
With 10 days left, ConnectiCare leads exchange sign-ups
ConnectiCare continues to lead the market among customers of Connecticut’s health insurance exchange, with 52 percent of the nearly 109,000 people signed up so far for 2016 coverage.
Anthem individual rates to rise 2.4%, ConnectiCare’s by 8.5%
Premiums for the 55,000 people who buy Anthem Blue Cross and Blue Shield health plans through the state’s individual market will rise by an average of 2.4 percent next year, while ConnectiCare Insurance Company’s 34,400 customers will see an average rate hike of 8.5 percent.
Regulator lowers most proposed health insurance rate hikes
Most insurance companies selling health plans in the state’s individual market will get to raise customers’ premiums in 2016, but not by as much as they proposed, and one major carrier will have to lower its rates, according to decisions released by the Connecticut Insurance Department Saturday.
Insurer coaches the newly covered through the health system
For those who gained coverage under Obamacare, learning to navigate the health care system can take more than an insurance card. This is the third in an occasional series of stories on health care issues in the wake of the Affordable Care Act.