Trying to pick a health plan? Wondering whether to buy the cheapest plan or the one with the most generous benefits? Are there other factors to consider?
We asked some experts for advice.
If you’re picking between plans offered through your job, skip ahead to item 2; the first one is intended for people who purchase their own plans through the state’s individual market.
This piece was originally published in 2013. It has been updated for 2016.
1. Where to look: Options on and off the exchange (for those who buy on their own).
People who purchase insurance on their own have two options: Buying plans through the state’s health insurance exchange or “off” the exchange.
The exchange, called Access Health CT, offers individual insurance policies sold by Anthem Blue Cross and Blue Shield and ConnectiCare. The exchange also offers plans to small businesses sold by Anthem.
Those companies, as well as insurers Aetna, Cigna and Golden Rule, also sell plans outside the exchange. People can buy those “off-exchange” plans through a broker or through an insurance company directly.
Why pick one option or the other?
People whose income falls below a certain mark (400 percent of the poverty level) can get a discount on their premiums if – and only if – they buy coverage through the exchange. The discount comes in the form of a federal tax credit, paid either in advance to the insurance company to supplement the customer’s premiums, or when the person files taxes for the year.
On the other hand, some plans sold outside the exchange are likely to have broader networks of health care providers. There are also more options available to people shopping outside the exchange.
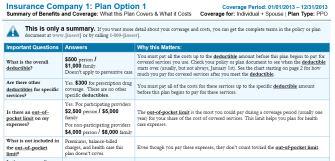
2. Get the “SBC” to compare apples to apples.
As part of the health reform law, the federal government requires all health insurers to make information about their plans available in a standardized, plain-language summary of benefits and coverage form, known an SBC.
The idea is to make it possible to easily compare plans. Shoppers can also request a glossary of terms used in health care coverage and medical care.
3. Price: What will it really cost you?
For many shoppers, cost is the top consideration in picking a plan, experts say. But they caution that it’s important for consumers to look at more than the premiums.
“It’s not just the price that they’re billed for,” said Kathy Walsh, principal examiner at the Connecticut Insurance Department’s consumer affairs division. “It’s also their out-of-pocket expenses. Sometimes it’s worth it to pay a little bit more for a plan that has less cost-sharing.”
Cost-sharing comes in the form of copayments – fixed dollar amounts, such as a $30 charge to see a primary care doctor – and coinsurance, in which people pay a fixed percentage of the cost of care.
Often, plans also have deductibles, which require members to pay a certain amount toward their medical costs before the insurance company will pay. In some plans, the deductible applies to nearly all services, while in others it’s limited to a few types of care. When weighing plans with deductibles, be sure you know what services are subject to the deductible, since differences in that factor can translate to major differences in your expenses.
Walsh advised people to think about how much medical care they typically use in a year and estimate what it would cost them under each plan they’re considering.
Access Health, the state’s health insurance exchange, is developing a tool intended to help people see the total costs they would face for each plan if they have certain medical conditions, counting both premiums and out-of-pocket costs for care. It was developed in response to concerns that many customers opted for the lowest-priced monthly premiums without realizing they would end up with deductibles that can top $10,000 for family coverage.
“Price doesn’t always equate to value, and that’s what I would be looking for,” state Healthcare Advocate Victoria Veltri said. “You can have a plan with a very low premium, but you may also have a $10,000 deductible and if you’re not walking around with a lot of cash in your pocket, it may not be providing a lot of value to you.”
Another number to pay attention to: The out-of-pocket maximum. That’s the most a member would have to spend on cost-sharing. Premiums don’t apply toward that number.
“That’s really your total liability and risk that you’re taking on,” said Tim Tracy, a Fairfield insurance broker and president of the Connecticut Chapter of the National Association of Health Underwriters.
4. Provider networks: Is your doctor covered? Do you need out-of-network benefits?
Experts advise consumers to make sure that any doctors or other providers they want to see are in the network for the plan they buy.
In some cases, the networks vary based on the plan, even within one insurance company. Anthem Blue Cross and Blue Shield and ConnectiCare have different networks for their exchange plans and their plans sold off the exchange, for example.
Because networks can change, Veltri recommended asking health care providers directly whether they participate with a plan, rather than relying on the insurer’s directory. And if you’re considering a plan sold through the exchange, be sure to ask the provider if they participate in the company’s exchange plan.
Another network-related issue to consider: How important is it to have coverage for care from providers who aren’t in the insurer’s network?
Some providers, such as psychologists and chiropractors, often don’t participate in insurer networks, Walsh noted. She suggested that people who want those types of services might want to consider plans that offer coverage for providers that aren’t in their network. In general, that’s more common among PPO or POS plans than in HMOs.
That’s also an important consideration for people who want coverage for care provided out-of-state, such as at hospitals in Boston or New York or the Mayo Clinic, Tracy said.
5. Are your medications covered and if so, what will they cost?
Different plans have their own list of drugs that will be covered, known as formularies, so people should make sure the plans they’re considering cover any medications they take, experts say.
Plans typically assign covered medications to specific tiers, and set patients’ cost-sharing for those drugs based on the tier. Even if a drug is covered by all plans, it might end up in different tiers for different plans, with potentially big cost differences.
6. Consider consulting an insurance broker.
The federal health law and creation of exchanges intended to allow people to comparison-shop for health plans led some people to think that the role of insurance brokers was diminishing. But brokers and consumer advocates said the changes associated with the health law and the complicated nature of picking insurance plans have reinforced the need for their help.
“The brokers who are stepping up are doing a really good job,” said Ellen Andrews, executive director of the Connecticut Health Policy Project.
Brokers get paid out of the money customers pay for their premiums, and the premiums are the same whether a person used a broker or not. That means that consumers won’t pay more for seeking their services. Brokers can also help out if clients have issues getting their coverage set up or run into issues with their coverage once they’ve purchased it.
But for exchange customers, beginning in 2017, Anthem and ConnectiCare will stop paying broker commissions. That means that people who want to buy a plan through Access Health might not be able to get help from an independent broker. Instead, the exchange plans to make some brokers available through its call center (855-805-4325).
That change does not apply to plans sold outside the exchange.
Tracy, the broker who advocates that people seek the advice of experts, said he recommends that people buying insurance ask questions.
“Because if you’re not asking questions and you’re just shopping based upon price, you could make a terrible, terrible mistake,” he said.