Taking a cue from concerns heard on the campaign trail and the stark disparities highlighted by the COVID-19 pandemic, lawmakers convened the 2021 session with lofty goals for health care reform in Connecticut.
Proposals on everything from cameras in nursing homes to government-sponsored insurance for small businesses and nonprofits were floated this session, with mixed success.
Among the bills that succeeded this year are a repeal of the state’s religious exemption from mandatory school vaccinations, a measure designed to boost health equity through better data collection and training, and an effort expanding the state’s Medicaid program, known as HUSKY, to undocumented children 8 years old and younger. But despite that, several substantial proposals failed to clear both chambers before the session adjourned on Wednesday.
Here’s a look at some of the key health reform bills that passed, passed with changes or failed during the 2021 regular session.

Bills that passed
Repeal of the religious exemption. For years, Democratic legislators have been pushing to erase Connecticut’s religious exemption from mandatory school vaccinations, citing concerns for immunocompromised children (who cannot be vaccinated for medical reasons). After two consecutive false starts, the proposal cleared both chambers and was signed into law by Gov. Ned Lamont. Under the new policy, the religious exemption will vanish beginning Sept. 1, 2022. Students in kindergarten through 12th grade who currently claim the exemption will be allowed to continue using it for the remainder of their academic careers, while those in pre-kindergarten, day care or who are new to the school system will no longer qualify.
Read more here, here, and here.
Health equity measures. Lawmakers adopted sweeping health equity reforms, including declaring racism a public health crisis in Connecticut, requiring better data collection on race and ethnicity in health care, mandating that hospitals conduct implicit bias training for employees who provide direct care to pregnant or postpartum women, requiring that the public health commissioner study the development of a recruitment and retention program for state health care workers who are people of color and directing the health department to explore whether to create a certification process for doulas.
Under an omnibus bill, legislators also voted to create a commission on racial equity in public health that would examine the impact of racism “on vulnerable populations within diverse groups … including on the basis of race, ethnicity, sexual orientation, gender identity and disability, including, but not limited to, Black American descendants of slavery.” The panel would be required to submit a report to the state’s Office of Policy and Management and to the Public Health and Appropriations committees by Jan. 1, 2022 and every six months thereafter outlining recommendations and documenting progress.
Read more about the changes here, here and here.
Ban on deceptive practices at pregnancy centers. The legislature took aim at so-called crisis pregnancy centers, religious facilities where critics say staff sometimes pose as medical professionals to lure women and hand out false information about abortions. The bill prohibits deceptive advertisements in print publications, online postings, public statements or “any other manner” and applies whether the centers do it themselves or someone else does it on their behalf. It also gives the Attorney General’s office the power to seek a court order to stop the deceptive practices. Lamont has signed the measure into law.
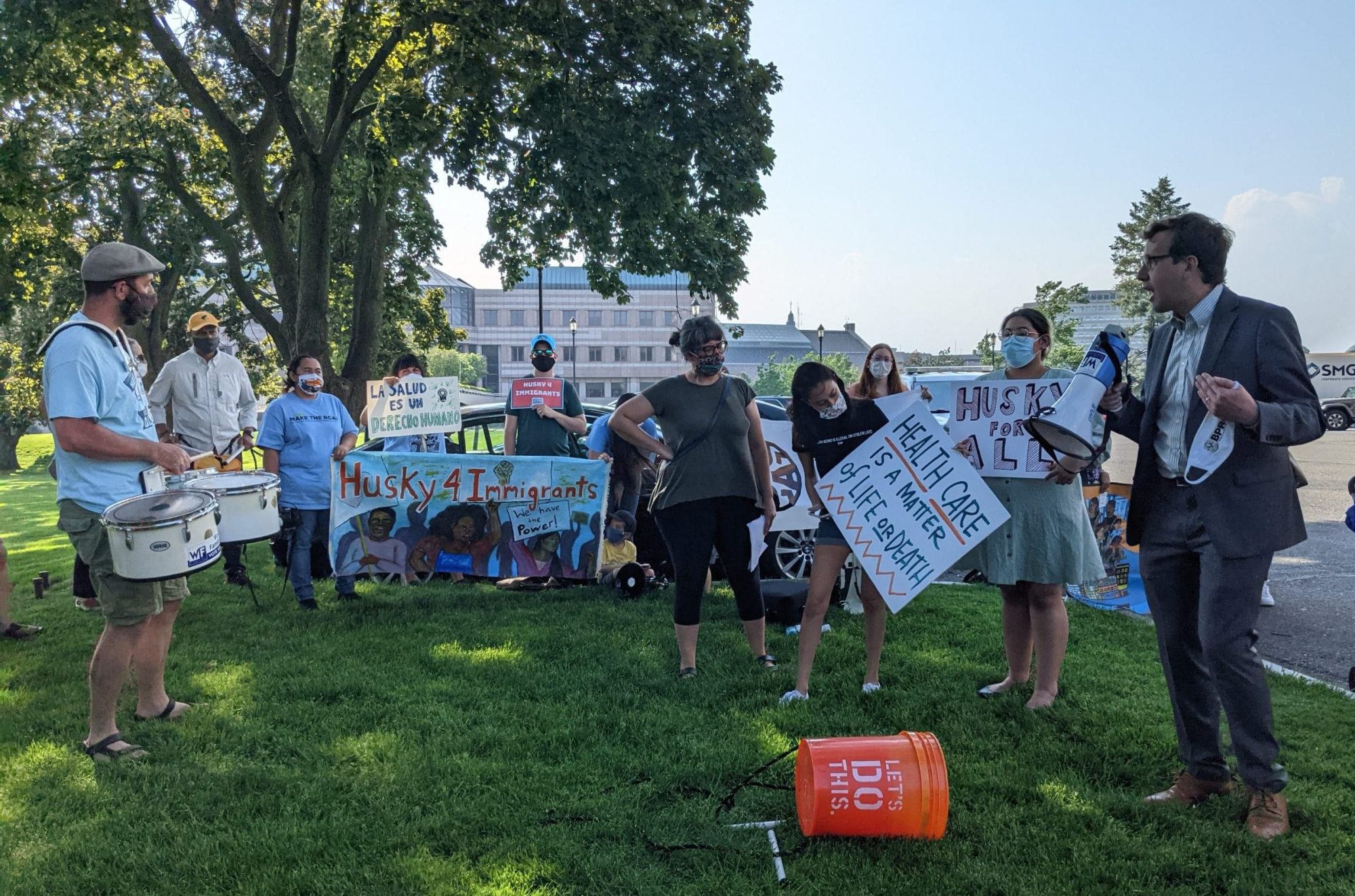
HUSKY for undocumented children. The General Assembly passed a last-minute bill opening the state’s Medicaid program, known as HUSKY, to children 8 and younger regardless of their immigration status. The expansion would begin on Jan. 1, 2023. Children from households earning up to 323% of the federal poverty level would qualify for the coverage. (That’s an income of $41,603 for a household of one, or $85,595 for a household of four.)
The bill also extends prenatal care to women, regardless of immigration status, whose household income is between 196% and 318% of the federal poverty level, and up to a year of postpartum care for women whose household income is at or below 263% of the FPL.
Additionally, the measure directs the Department of Social Services to study the feasibility of extending HUSKY coverage to children, regardless of immigration status, from ages 9 to 18, and to adults whose households earn up to 200% of the FPL.
Lamont has not yet signed the bill.
Read more here.
Some nursing home changes. Legislators passed bills that permit the use of cameras and other technology in nursing homes, strengthen the so-called bill of rights for residents by adding that they have the right to treat their living quarters as their own home, and allow residents of long-term care facilities to designate an “essential support person” who may enter a nursing home in spite of visitor restrictions. Proponents had pushed for those measures after more than 3,800 people died in nursing homes and went months without seeing loved ones during the COVID-19 pandemic.
The legislature also approved a wide-ranging proposal that increases minimum staffing hours, to 3 hours of direct care per resident per care, up from 1.9. The bill also requires all nursing homes to employ a full-time infection prevention specialist and to maintain at least a two-month supply of personal protective gear.

Dental and vision coverage for young adults. Young adults, stepchildren and other dependent children will be able to remain on their parents’ dental and vision insurance through age 26 under a bill that cleared both chambers.
While the Affordable Care Act allows young adults to stay on their parents’ insurance through age 26, the same is not always true for dental and vision coverage. Pediatric care, including vision and dental, are considered an essential health benefit under the ACA and are covered through age 19. Some employer-sponsored plans can choose to insure children beyond that, but many don’t, health officials say.
The measure applies to fully insured plans, such as those on the exchange, and ensures that children can remain on their parents’ dental and vision coverage even if they are offered plans through their employer.
Read more here.
Telehealth. The legislature authorized an extension of an executive order loosening restrictions on telemedicine appointments, which have become vital for many patients during the COVID-19 pandemic.
The measure allows health care providers and patients to communicate over a broader range of platforms, including audio-only phone calls. Under the mandate, a greater variety of health care professionals can also conduct the visits, from behavioral therapists to dentists.
The bill also ensures payment parity, meaning insurers would have to pay providers the same amount for a telehealth visit as they would for an in-person appointment. The bill would keep the changes in place through June 30, 2023.

Bills that failed or passed with changes
Public option. For three consecutive years, lawmakers have tried unsuccessfully to expand government-sponsored health insurance. The latest version of the public option bill would have extended that coverage to small businesses and nonprofits. The measure included several other health care reform proposals, such as an expansion of HUSKY and an assessment on insurance carriers that would fund additional subsidies on the state’s health insurance exchange. Many of those other provisions also died.
Some nursing home changes. While several nursing home reforms were approved this session, advocates had hoped for a more extensive overhaul in certain areas.
One of those is minimum staffing. While the General Assembly approved raising the minimum hours of direct care per resident per day from 1.9 to three, proponents had hoped for 4.1 hours. Lawmakers and the state’s Office of Fiscal Analysis said the move would have cost hundreds of millions of dollars, so a proposal was amended to require three hours of direct care per resident per day.
Read more here.
Assessment on insurers. When the public option bill died, lawmakers had considered including an assessment on insurance carriers in the state budget. They ultimately did not. The assessment would have brought in up to $50 million per year, and the money would have been used for a variety of initiatives, including enhanced subsidies on the exchange, an expansion of HUSKY to more Connecticut residents, and a reinsurance program.
Prescription drug cap. Lamont had proposed capping annual increases in the cost of prescription drugs. His measure would have limited yearly hikes by drug manufacturers to the rate of inflation plus 2%. Pharmaceutical companies that exceeded that amount would have gotten hit with a fine.
The plan ran into trouble as the session went on. Legislators said it would be difficult to impose the cap on companies like Pfizer, which have developed life-saving COVID-19 vaccines.

Aid in dying. For the first time ever, a bill that would let terminally ill patients access medication to end their lives was voted out of the Public Health Committee this year. The measure had never made it past that crucial hurdle, and this spring it did so with bipartisan support. Despite that, it failed to win passage in the Judiciary Committee and didn’t come up for a vote in either the House or the Senate.
Under the proposal, an adult patient with a terminal illness – having six months or less to live – would have been able to access lethal drugs by making two oral requests at least 15 days apart, and one written request. The written request must be done in the presence of two witnesses who can attest that the patient is of sound mind and acting voluntarily.
A physician would have prescribed or dispensed the medication, and the patient would have self-administered the drug. Requests for the medication could have been rescinded by the patient at any time “without regard to his or her mental state,” according to the measure.
Read more here.
Health care sharing ministries. Legislators considered a bill that would have barred insurance agents and brokers from marketing and selling plans run by health care sharing ministries, nonprofit religious organizations that pool their members’ contributions with the intent of paying out medical bills, though there is often no guarantee of coverage.
As the health ministries have gained popularity in recent years, drawing new members by marketing themselves as a lower-cost alternative to traditional health insurance, grievances have also multiplied against the groups. Connecticut residents who are members of the organizations have complained about denial of coverage and non-payment of medical bills. Some say they were duped into buying the plans, believing they were purchasing health insurance. Others said they were aware the ministries were not traditional coverage but still expected all of their medical bills to be paid – only to find out they weren’t.

The bill would have prohibited anyone licensed by the state’s insurance department from conducting business with a health care sharing ministry. It also would have barred everyone – regardless of their position – from accepting money for selling or marketing a ministry plan to Connecticut residents, for negotiating such a plan on behalf of a resident, or for administering such a plan that includes any state resident.
The proposal made it through the Insurance and Real Estate Committee but did not come up for a vote in the House or Senate.
Read more here, here and here.
Coverage for adults and older children who are undocumented. A bill that would have extended HUSKY coverage to people regardless of their immigration status did not come up for debate in the House or Senate, despite passing through the Human Services and Appropriations committees. Under the measure, residents would have had to meet the qualifying household income limits to be eligible for the coverage (those limits differ for the various programs – HUSKY A, B, C, and D). Advocates stood outside the state Capitol throughout the session rallying for passage of the bill. But the bill had a large fiscal note – costing $67 million to $116 million during the first year and $200 million to $258 million the second year.